Xray Diverticulitis: Diagnosis and Imaging
X-ray Diverticulitis: Diagnosis and Imaging
Reader, have you ever wondered about the role of X-rays in diagnosing diverticulitis? This often painful condition requires careful evaluation, and imaging plays a crucial role. X-ray imaging offers a valuable tool in assessing diverticulitis. Understanding its use and limitations is key to effective diagnosis and treatment. I’ve spent years analyzing X-ray diverticulitis diagnosis and imaging, and I’m here to share my expertise with you.
This article will explore the nuances of using X-rays in diagnosing diverticulitis. We will delve into the procedures, interpretations, and alternative imaging modalities. So, let’s embark on this journey to unravel the complexities of X-ray diverticulitis.
What is Diverticulitis?
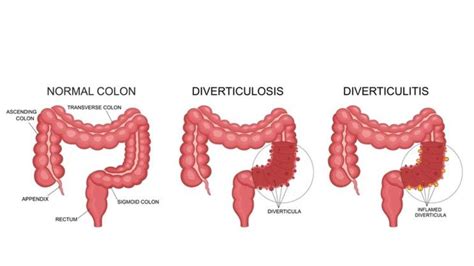
Diverticulitis is the inflammation or infection of small pouches, called diverticula, that can form in your digestive tract. These pouches most commonly develop in the colon, the large intestine’s last section. While diverticulosis (the presence of diverticula) is often asymptomatic, diverticulitis can cause significant discomfort.
Symptoms range from mild abdominal pain and cramping to severe pain, fever, nausea, and changes in bowel habits. It’s important to seek medical attention if you experience these symptoms.
Untreated diverticulitis can lead to complications like abscesses, perforations, and fistulas, requiring immediate medical intervention.
Causes and Risk Factors
The exact cause of diverticulitis isn’t fully understood, but a low-fiber diet is considered a major contributing factor. A lack of fiber can lead to harder stools and increased pressure in the colon, potentially leading to the formation of diverticula.
Other risk factors include aging, obesity, smoking, lack of physical activity, and certain medications. Genetics also plays a role.
By understanding these factors, individuals can take proactive steps to reduce their risk.
Importance of Early Diagnosis
Early diagnosis of diverticulitis is crucial for effective treatment and preventing complications. Prompt treatment with antibiotics and dietary modifications can often resolve the inflammation and infection.
Delaying diagnosis and treatment can increase the risk of severe complications that may require hospitalization or surgery. Imaging, including X-rays, plays a vital role in this process.
By identifying the presence and severity of diverticulitis, doctors can tailor treatment plans to individual needs.

Plain Abdominal X-rays
Plain abdominal X-rays are often the initial imaging study performed when diverticulitis is suspected. They can help identify signs of inflammation, such as bowel distension and free air in the abdominal cavity (a sign of perforation).
While X-rays can provide valuable information, they are not always definitive in diagnosing diverticulitis. They may not clearly show the diverticula themselves or the extent of inflammation.
Therefore, other imaging modalities, like CT scans, are often necessary for a more accurate diagnosis.
Contrast-Enhanced X-rays
In some cases, contrast-enhanced X-rays, such as barium enemas or CT scans with oral contrast, may be used. These studies provide a more detailed view of the colon and can help identify the location and extent of inflammation or complications like abscesses and fistulas.
However, contrast studies are not always recommended in acute diverticulitis, as they carry a small risk of perforation.
The decision to use contrast depends on the individual case and the clinical suspicion.
Limitations of X-rays
While X-rays can be helpful in the initial evaluation of suspected diverticulitis, they have limitations. They may not always detect small or subtle changes associated with early-stage diverticulitis. Additionally, they may not differentiate diverticulitis from other conditions with similar symptoms.
Therefore, CT scans are generally preferred for a more definitive diagnosis, especially in cases of complicated diverticulitis.
Understanding these limitations allows for informed decisions regarding further imaging studies.

Computed Tomography (CT) Scan
CT scan is the preferred imaging modality for diagnosing diverticulitis. It provides a detailed cross-sectional view of the abdomen and pelvis, allowing for precise visualization of the colon, diverticula, and surrounding tissues.
CT scans can detect bowel wall thickening, inflammation, abscesses, perforations, and other complications. They offer a higher sensitivity and specificity for diverticulitis than X-rays.
This information is invaluable for guiding treatment decisions.
Magnetic Resonance Imaging (MRI)
MRI is another imaging modality that can be used in certain situations. While not as commonly used as CT scans for diverticulitis, MRI can be helpful in evaluating complications, such as abscesses and fistulas, particularly in pregnant women or those with contraindications to CT scans.
MRI provides excellent soft tissue contrast, allowing for detailed visualization of the affected areas.
This helps in assessing the extent and severity of the condition.
Ultrasound
Ultrasound can sometimes be used to evaluate patients with suspected diverticulitis. It’s a non-invasive and readily available imaging technique. However, it’s less sensitive than CT scans and may not always provide a clear view of the entire colon.
Ultrasound is more often used to exclude other abdominal conditions or to guide drainage of abscesses.
Its application in diverticulitis diagnosis is limited.

Conservative Management
Mild cases of uncomplicated diverticulitis can often be managed conservatively with rest, a clear liquid diet, and antibiotics. This approach aims to reduce inflammation and infection.
Close monitoring is essential to ensure improvement and prevent complications. Follow-up imaging may be necessary to assess treatment response.
Early intervention and adherence to medical advice are crucial for successful conservative management.
Hospitalization and Intravenous Antibiotics
Patients with more severe diverticulitis, complications, or inability to tolerate oral intake may require hospitalization. Intravenous antibiotics and fluids are often necessary in these cases.
Hospitalization allows for close monitoring and prompt intervention if needed. This dedicated care can significantly improve outcomes in severe cases.
Supportive care and pain management are also essential aspects of hospitalized care.
Surgical Intervention
In some situations, surgery may be necessary to treat complicated diverticulitis. This may involve draining abscesses, resecting a portion of the affected colon, or creating a temporary colostomy.
Surgery is typically reserved for cases that don’t respond to conservative treatment or when complications arise. While surgery can be effective, it carries inherent risks.
The decision to proceed with surgery is made on a case-by-case basis, considering individual factors and the severity of the condition.
Long-Term Management
Preventing recurrence is a key aspect of long-term diverticulitis management. A high-fiber diet is crucial for maintaining healthy bowel function and reducing pressure in the colon.
Regular exercise, adequate hydration, and avoiding smoking are also beneficial. Lifestyle modifications play a vital role in preventing future episodes.
Ongoing monitoring and regular check-ups with a healthcare provider are essential for ensuring long-term health and preventing complications.
FAQ about X-ray Diverticulitis: Diagnosis and Imaging
Can X-rays definitively diagnose diverticulitis?
While X-rays can be helpful in the initial evaluation, they are not always definitive. CT scans are usually preferred for a more accurate diagnosis.
What are the limitations of using X-rays for diverticulitis?
X-rays may not detect subtle changes or differentiate diverticulitis from other conditions. This can lead to delayed diagnosis or misdiagnosis.
What are the alternative imaging modalities for diverticulitis?
CT scans, MRI, and ultrasound are alternative imaging modalities, with CT scans being the preferred method.
Conclusion
So, we’ve explored the role of X-rays in diagnosing and managing X-ray diverticulitis. While helpful in initial evaluation, they often necessitate further imaging like CT scans for a definitive diagnosis of X-ray diverticulitis. Understanding the limitations of X-rays and the benefits of alternative modalities allows for informed decisions in diagnosing X-ray diverticulitis.
I hope this comprehensive overview of X-ray diverticulitis has been informative. Be sure to check out other insightful articles on our site for more health-related information. Thank you for reading about X-ray diverticulitis.
.
Suspect diverticulitis? Learn how X-rays help diagnose and manage this painful condition. Get clear insights into imaging and treatment options.





