Que Causa La Diverticulitis: Causes & Risk Factors
What Causes Diverticulitis: Causes & Risk Factors
Reader, have you ever wondered what causes diverticulitis, a condition affecting millions worldwide? It’s crucial to understand the underlying causes and risk factors associated with this often painful digestive disorder. Diverticulitis can range from mild discomfort to a serious medical emergency. Knowing the causes empowers you to make informed choices for better digestive health. As an experienced health writer, I’ve analyzed extensive research on the causes and risk factors of diverticulitis to provide you with valuable insights.
This comprehensive guide delves deep into the intricacies of diverticulitis, exploring everything from dietary influences to genetic predispositions. Understanding these factors is the first step toward prevention and effective management. Let’s embark on this journey to unravel the mysteries of what causes diverticulitis.
What is Diverticulitis?
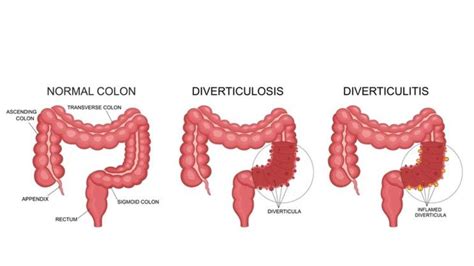
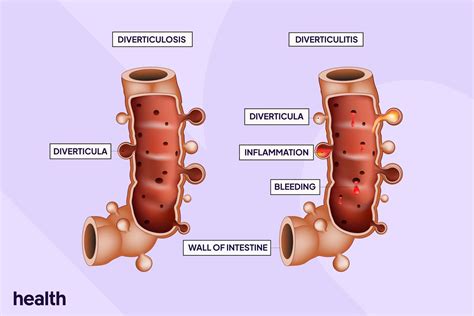
Diverticulitis is the inflammation or infection of diverticula, small bulging pouches that can form in the lining of your digestive system. These pouches are most common in the lower part of the large intestine (colon). Diverticulitis occurs when these pouches become inflamed or infected.
This can lead to a range of symptoms, from mild abdominal pain to severe complications like abscesses or perforations. Understanding the difference between diverticulosis (the presence of diverticula) and diverticulitis (inflammation of diverticula) is key.
While most people with diverticulosis never experience any symptoms, a small percentage develop diverticulitis. It’s important to be aware of the potential risks and take steps to maintain a healthy digestive system.
Symptoms of Diverticulitis
Diverticulitis symptoms can vary from mild to severe. The most common symptom is abdominal pain, typically on the lower left side. This pain can be constant or intermittent.
Other symptoms can include fever, chills, nausea, vomiting, constipation, or diarrhea. Changes in bowel habits are also common, such as alternating between constipation and diarrhea.
If you experience any of these symptoms, it’s important to seek medical attention. Prompt diagnosis and treatment can help prevent complications.
The Role of Diet in Diverticulitis
A low-fiber diet is considered a primary risk factor for developing diverticula, which can then become inflamed and lead to diverticulitis. Fiber adds bulk to the stool, making it easier to pass and reducing pressure on the colon walls.
When the stool is hard and small due to a lack of fiber, the colon has to work harder to push it through. This increased pressure can cause weak spots in the colon wall to bulge out, forming diverticula.
Consuming a high-fiber diet rich in fruits, vegetables, and whole grains can help prevent diverticulitis by promoting regular bowel movements and reducing pressure on the colon.
Genetic Predisposition to Diverticulitis
While diet plays a significant role, genetics also contribute to the development of diverticulitis. If you have a family history of the condition, you may be at a higher risk.
Research suggests that certain genes may influence the structure and strength of the colon wall, making some individuals more susceptible to developing diverticula. Although genetic factors can’t be controlled, it is important to be aware of the increased risk.
This knowledge empowers you to make proactive lifestyle choices, such as adopting a high-fiber diet and maintaining a healthy weight, to mitigate the risk of diverticulitis.
Other Contributing Factors to Diverticulitis
Beyond diet and genetics, other factors like aging, lack of exercise, smoking, and certain medications can contribute to diverticulitis. As we age, the colon wall naturally weakens, increasing the risk of diverticula formation.
Regular exercise supports overall digestive health and promotes regular bowel movements, reducing pressure on the colon. Smoking weakens the colon wall and increases inflammation, raising the risk of diverticulitis.
Certain medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs), can also irritate the colon and increase the risk of diverticulitis. Consulting with your doctor about potential medication interactions is always a good idea.

Age and Diverticulitis
Age is a significant risk factor for diverticulitis. Diverticula are more common in older adults, with the prevalence increasing significantly after age 40. As we age, the colon wall loses some of its elasticity and strength, making it more susceptible to the formation of diverticula.
While diverticula can occur in younger people, they are much less common. The majority of diverticulitis cases occur in individuals over 60. Maintaining a healthy lifestyle, especially focusing on a high-fiber diet, becomes increasingly important with age to reduce the risk of diverticulitis.
Staying active and hydrated can also support digestive health and reduce the risk of complications as you age.
Obesity and Diverticulitis
Being overweight or obese increases the risk of developing diverticulitis. Excess weight, especially around the abdomen, puts added pressure on the digestive system. This increased pressure can contribute to the formation of diverticula.
Maintaining a healthy weight through a balanced diet and regular exercise is crucial for reducing the risk of diverticulitis. Weight management not only reduces pressure on the colon but also supports overall health and well-being.
Adopting healthy lifestyle choices is key to preventing diverticulitis and maintaining long-term digestive health.
Lack of Exercise and Its Impact on Diverticulitis
Regular physical activity plays an important role in preventing diverticulitis. Exercise promotes regular bowel movements, which helps reduce pressure on the colon and prevent constipation. A sedentary lifestyle increases the risk of developing diverticula and subsequent diverticulitis.
Aim for at least 30 minutes of moderate-intensity exercise most days of the week. Activities like brisk walking, swimming, or cycling can help keep your digestive system healthy. Incorporating regular exercise into your routine not only benefits your digestive health but also improves overall well-being.
It can contribute to weight management, reduce stress, and improve cardiovascular health – all factors that indirectly impact the risk of diverticulitis.
Detailed Breakdown of Diverticulitis Causes and Risk Factors
| Factor | Description | Impact on Diverticulitis |
|---|---|---|
| Low-Fiber Diet | A diet lacking in fruits, vegetables, and whole grains. | Increases the risk of diverticula formation and subsequent diverticulitis due to increased pressure on the colon. |
| Genetic Predisposition | Family history of diverticulitis. | Increases susceptibility to developing diverticula. |
| Age | Increasing age, particularly over 40. | Weakening of the colon wall increases the risk of diverticula formation. |
| Obesity | Excess weight, particularly around the abdomen. | Adds pressure on the digestive system, promoting diverticula formation. |
| Lack of Exercise | Sedentary lifestyle. | Contributes to constipation and increases pressure on the colon. |
FAQ: Frequently Asked Questions about Diverticulitis
What is the difference between diverticulosis and diverticulitis?
Diverticulosis is the presence of diverticula (small pouches in the colon wall), while diverticulitis is the inflammation or infection of these pouches.
Many people with diverticulosis never experience any symptoms. Diverticulitis, on the other hand, can cause abdominal pain, fever, and other digestive issues.
It’s important to distinguish between these two conditions to ensure proper management and prevention.
Can diverticulitis be prevented?
While not entirely preventable, the risk of diverticulitis can be significantly reduced through lifestyle modifications. A high-fiber diet, regular exercise, maintaining a healthy weight, and staying hydrated are key preventative measures.
These lifestyle choices contribute to regular bowel movements and reduce pressure on the colon, minimizing the likelihood of developing diverticula and subsequent inflammation.
Consulting with a healthcare professional can provide personalized guidance on managing risk factors.
.





