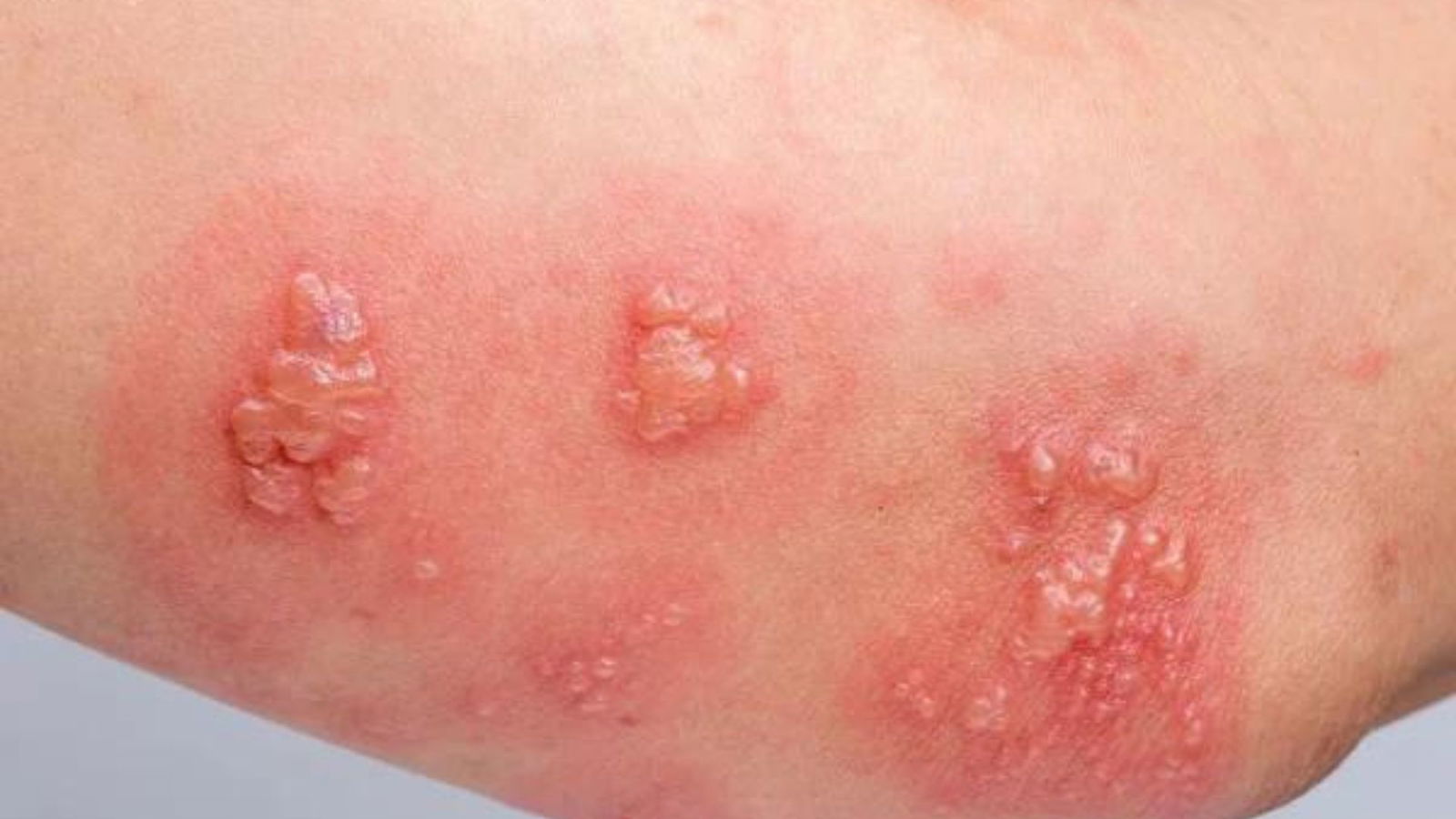
Juvenile Psoriasis: Treatment and Support
Juvenile Psoriasis: Treatment and Support
Reader, have you ever wondered about the challenges of managing juvenile psoriasis? It’s a skin condition that can significantly impact a child’s life. Juvenile psoriasis is more than just a skin deep issue; it’s a complex condition demanding specialized care. Navigating the treatment landscape can feel overwhelming for both parents and children. I have years of experience analyzing juvenile psoriasis and have compiled comprehensive information to help you understand and manage this condition.
Juvenile psoriasis is a chronic autoimmune disease that manifests on the skin. Characterized by red, scaly patches, it can range from mild to severe. Understanding the nuances of this condition is crucial for effective management and support.
Understanding Juvenile Psoriasis
What is Juvenile Psoriasis?
Juvenile psoriasis is a chronic skin condition affecting children and adolescents. It causes skin cells to grow too quickly, resulting in thick, scaly patches. These patches are often red, itchy, and sometimes painful. This form of psoriasis can significantly impact a child’s quality of life.
Early diagnosis and appropriate treatment are crucial for managing the condition. This can help minimize the physical and emotional impact on young patients.
Recognizing the symptoms and seeking professional help can lead to a better outcome for affected children. Support from family and healthcare professionals is essential.
Types of Juvenile Psoriasis
Several distinct types of juvenile psoriasis exist, each with its own characteristics. Plaque psoriasis is the most common, characterized by raised, red patches covered with silvery scales. Guttate psoriasis appears as small, drop-shaped lesions, often triggered by a strep throat infection.
Inverse psoriasis occurs in skin folds, while pustular psoriasis presents with pus-filled blisters. Erythrodermic psoriasis, the rarest and most severe form, covers the entire body with redness and scaling. Understanding these different types is vital for tailored treatment.
Each type requires a specific approach to management. Consulting with a dermatologist is essential for proper diagnosis and treatment planning.
Juvenile Psoriasis: Treatment Options
Topical Treatments
Topical treatments are often the first line of defense against juvenile psoriasis. These include corticosteroids, vitamin D analogs, and coal tar preparations. These medications help reduce inflammation and slow skin cell growth.
Choosing the right topical treatment depends on the severity and location of the psoriasis. A dermatologist can help determine the most suitable option for each child.
Proper application techniques are essential for maximizing effectiveness and minimizing side effects. Parents should receive clear instructions on how to apply the prescribed medications.
Systemic Medications
For moderate to severe juvenile psoriasis, systemic medications may be necessary. These medications work throughout the body to control the immune system and reduce inflammation. Examples include methotrexate, cyclosporine, and biologics.
Systemic treatments are typically reserved for cases where topical treatments are insufficient. These medications can have potential side effects, requiring careful monitoring.
Regular blood tests and check-ups are essential to ensure the safety and efficacy of systemic treatments. Close collaboration with a dermatologist is crucial.
Phototherapy
Phototherapy involves exposing the skin to controlled amounts of ultraviolet (UV) light. This can help slow down skin cell growth and reduce inflammation in juvenile psoriasis. Different types of phototherapy exist, including UVB and PUVA.
Phototherapy sessions are typically conducted under the supervision of a dermatologist. The frequency and duration of treatment vary depending on the individual’s needs.
Protecting the eyes and other sensitive areas during phototherapy is essential. Patients should follow the dermatologist’s instructions carefully.
Living with Juvenile Psoriasis: Support and Resources
Emotional Support
Living with juvenile psoriasis can be emotionally challenging for children. The visible nature of the condition can lead to self-consciousness and social anxiety. Providing emotional support is crucial for their well-being.
Connecting children with support groups and counseling services can be beneficial. Open communication within the family is also essential.
Helping children develop coping mechanisms and build self-esteem can empower them to manage their condition. Encouraging participation in activities they enjoy can also be helpful.
Practical Tips for Managing Juvenile Psoriasis
Several practical tips can help manage juvenile psoriasis effectively. Maintaining a healthy lifestyle, including a balanced diet and regular exercise, can improve overall health and skin condition. Avoiding triggers, such as stress and certain infections, can also help minimize flare-ups.
Keeping the skin moisturized is essential to prevent dryness and itching. Using gentle, fragrance-free skincare products is recommended. Protecting the skin from excessive sun exposure is also important.
Educating family members, friends, and school staff about juvenile psoriasis can promote understanding and support. This can help create a more inclusive environment for the child.
Resources and Organizations
Numerous resources and organizations provide valuable information and support for individuals with juvenile psoriasis. The National Psoriasis Foundation offers educational materials, support groups, and online forums. The American Academy of Dermatology provides expert guidance on diagnosis and treatment.
Local support groups can offer a sense of community and connection. Connecting with other families facing similar challenges can be incredibly helpful. Online forums can provide a platform for sharing experiences and seeking advice.
Utilizing these resources can empower individuals and families to effectively manage juvenile psoriasis. Staying informed about the latest research and treatment options is crucial.
Detailed Breakdown of Treatment Options for Juvenile Psoriasis
| Treatment Type | Description | Benefits | Potential Side Effects |
|---|---|---|---|
| Topical Corticosteroids | Reduce inflammation and itching | Effective for mild to moderate psoriasis | Skin thinning, discoloration |
| Vitamin D Analogs | Slow skin cell growth | Safe for long-term use | Skin irritation |
| Coal Tar | Reduces scaling and inflammation | Cost-effective | Strong odor, staining |
| Methotrexate | Suppresses the immune system | Effective for moderate to severe psoriasis | Liver damage, nausea |
| Biologics | Targets specific immune system pathways | Highly effective for severe psoriasis | Increased risk of infections |
| UVB Phototherapy | Slows skin cell growth | Effective for widespread psoriasis | Sunburn, premature aging |
| PUVA Phototherapy | Combines UVA light with a medication | Effective for resistant psoriasis | Nausea, increased risk of skin cancer |
Frequently Asked Questions about Juvenile Psoriasis
What triggers juvenile psoriasis?
Several factors can trigger or worsen juvenile psoriasis, including infections, stress, skin injuries, and certain medications. Identifying and managing these triggers can help reduce flare-ups. It’s important to consult with a dermatologist to determine individual triggers.
Keeping a journal to track potential triggers can be helpful. This can provide valuable insights into what might be exacerbating the condition.
Working with a healthcare professional to develop a personalized trigger management plan is essential.
Is juvenile psoriasis contagious?
Juvenile psoriasis is not contagious. It is an autoimmune condition, meaning it’s caused by the body’s immune system attacking healthy skin cells. It cannot be spread from person to person through physical contact.
Educating others about the non-contagious nature of psoriasis can help reduce stigma and misconceptions. This can create a more supportive environment for children with psoriasis.
Encouraging open communication and understanding within social circles can significantly benefit affected children.
How can I support my child with juvenile psoriasis?
Providing emotional support, encouraging open communication, and connecting them with resources can make a significant difference. Creating a supportive and understanding environment at home and school can help children cope with the challenges of living with this condition.
Empowering children to take an active role in managing their condition can foster a sense of control and improve their overall well-being. This can include teaching them about their treatment plan and how to identify triggers.
Celebrating their strengths and resilience can build self-esteem and help them navigate the emotional impact of juvenile psoriasis.
Conclusion
So, understanding juvenile psoriasis is the first step towards effective management and support. From diagnosis to various treatment options and valuable resources, this guide aims to empower you with the knowledge needed to navigate this journey. Remember, early intervention and consistent care are key to improving the quality of life for children with juvenile psoriasis.
We’ve covered a lot about juvenile psoriasis. Be sure to check out other informative articles on our site to learn more about related health topics. Managing juvenile psoriasis is a continuous process, and staying informed is essential for ongoing success. Early diagnosis and consistent care are vital for improving the quality of life for children with this condition.
.
Effective treatments & support for juvenile psoriasis. Manage symptoms, boost confidence. Find info on medications, therapies, and support groups.