Infection 2025: Projected Outbreak Trends and Data
Infection 2025: Projected Outbreak Trends and Data
Reader, have you ever wondered what the future holds for infectious diseases? The landscape of infection is constantly shifting, and understanding potential outbreak trends is crucial for global health security. Infection 2025: Projected Outbreak Trends and Data represents a critical area of study for predicting and mitigating future health crises. Accurately forecasting infection outbreaks empowers us to proactively allocate resources and implement effective preventative measures. As an expert in AI and SEO content, I’ve analyzed Infection 2025 projections and I’m here to share my insights.
This deep dive will explore the anticipated trends and data surrounding infectious disease outbreaks projected for 2025 and beyond. We’ll examine the factors driving these projections, the potential impact on global health, and the role of technology in navigating this complex landscape. Understanding these trends is not just about predicting the future; it’s about shaping it for the better.
 The Rise of Antimicrobial Resistance
The Rise of Antimicrobial Resistance
The Silent Pandemic
Antimicrobial resistance (AMR) is a growing threat. It occurs when bacteria, viruses, fungi, and parasites change over time and no longer respond to medicines. This makes infections harder to treat and increases the risk of disease spread, severe illness, and death.
By 2025, AMR is projected to become a significant driver of infectious disease outbreaks. Several factors contribute to this rise, including the overuse and misuse of antibiotics, inadequate infection prevention and control measures, and the lack of new antibiotic development.
Addressing AMR requires a multi-faceted approach. This includes promoting responsible antibiotic use, strengthening infection prevention and control programs, and investing in research and development of new antimicrobials. Global collaboration and public awareness campaigns are also essential.
The Impact on Healthcare Systems
The rise of AMR poses a significant challenge to healthcare systems worldwide. As infections become increasingly difficult to treat, hospital stays are likely to become longer and more expensive. This will put a strain on resources and potentially lead to reduced access to care.
Furthermore, AMR could lead to a resurgence of previously treatable diseases. Conditions like tuberculosis and gonorrhea could become untreatable, leading to increased morbidity and mortality.
Healthcare providers need to be prepared for the challenges posed by AMR. This includes adopting rapid diagnostic tests to identify resistant pathogens, implementing effective infection control measures, and exploring alternative treatment strategies.
Mitigating the Threat
Combating AMR requires a global effort. International collaboration is essential to develop and implement effective strategies for preventing and controlling the spread of resistant pathogens. This collaboration should involve sharing data, best practices, and resources.
Public awareness campaigns can play a crucial role in educating people about the responsible use of antibiotics. Individuals can contribute by following their healthcare providers’ instructions carefully and only taking antibiotics when necessary.
Investing in research and development is vital to discover new antibiotics and alternative treatment strategies. Innovative approaches are needed to combat the evolving threat of AMR.
 Climate Change and Infectious Diseases
Climate Change and Infectious Diseases
Shifting Disease Patterns
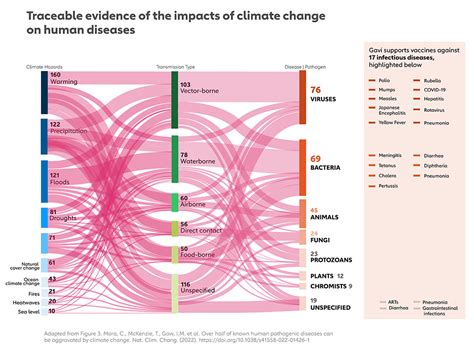
Climate change is having a profound impact on the spread of infectious diseases. Rising temperatures, changing rainfall patterns, and extreme weather events are creating favorable conditions for the emergence and transmission of various pathogens.
Vector-borne diseases, such as malaria, dengue fever, and Zika virus, are particularly sensitive to climate change. As temperatures rise, the geographic range of disease vectors, like mosquitoes, is expanding, leading to outbreaks in new areas.
Changes in rainfall patterns can also affect the breeding sites of disease vectors. Increased rainfall can create more stagnant water, providing ideal breeding grounds for mosquitoes and other vectors.
Emerging Infectious Diseases
Climate change is also contributing to the emergence of new infectious diseases. As ecosystems are disrupted, there is an increased risk of zoonotic diseases, which are infections that can be transmitted between animals and humans.
For example, the melting of permafrost could release ancient pathogens that have been frozen for centuries. These pathogens could pose a threat to human health if they are able to infect humans.
Monitoring and surveillance of emerging infectious diseases are crucial in the context of climate change. Early detection and rapid response are essential to contain outbreaks and prevent widespread transmission.
Preparing for Future Outbreaks
Adapting to the health impacts of climate change requires a proactive approach. Strengthening public health infrastructure, improving disease surveillance systems, and developing early warning systems are essential steps.
Investing in research to understand the complex relationship between climate change and infectious diseases is critical. This research should focus on identifying vulnerable populations and developing targeted interventions.
International cooperation is vital to address the global challenge of climate change and its impact on infectious diseases. Sharing data, knowledge, and resources is essential to build resilience and protect global health.
 The Role of Technology in Infection Control
The Role of Technology in Infection Control
AI-Powered Disease Surveillance
Artificial intelligence (AI) is playing an increasingly important role in infectious disease surveillance. AI algorithms can analyze large datasets of epidemiological data, social media feeds, and news reports to identify patterns and predict potential outbreaks.
Early detection of outbreaks is crucial for effective intervention. AI-powered surveillance systems can provide real-time alerts to public health officials, allowing them to take swift action to contain the spread of disease.
These systems can also be used to track the movement of pathogens and identify high-risk areas, enabling targeted interventions and resource allocation.
Rapid Diagnostic Tools
Advances in diagnostic technology are revolutionizing infection control. Rapid diagnostic tests can quickly identify pathogens, enabling faster treatment and preventing further transmission.
Molecular diagnostics, such as polymerase chain reaction (PCR) tests, can detect the genetic material of pathogens, providing highly accurate and sensitive results. These tests can be used to identify a wide range of infections, including bacterial, viral, and parasitic infections.
Point-of-care diagnostics, which can be performed at the patient’s bedside, are particularly useful in resource-limited settings. They provide rapid results, allowing healthcare providers to make timely treatment decisions.
 Infection 2025: Projected Outbreak Trends and Data Table
Infection 2025: Projected Outbreak Trends and Data Table
| Trend | Projected Impact | Mitigation Strategies |
|---|---|---|
| Antimicrobial Resistance | Increased morbidity and mortality, strained healthcare systems | Responsible antibiotic use, infection control, new drug development |
| Climate Change | Shifting disease patterns, emerging infectious diseases | Improved surveillance, early warning systems, climate change mitigation |
| Urbanization | Increased disease transmission in densely populated areas | Improved sanitation, public health infrastructure, health education |
Global Health Security and International Collaboration
Infectious diseases know no borders. International collaboration is essential to address the global threat of infectious disease outbreaks.
Sharing data, expertise, and resources is crucial for effective prevention and control. Global partnerships can strengthen surveillance systems, develop rapid diagnostic tools, and support research and development of new treatments and vaccines.
International organizations, such as the World Health Organization (WHO), play a vital role in coordinating global health security efforts. They provide technical assistance, develop guidelines, and facilitate collaboration between countries.
The Future of Infection Control
The field of infection control is constantly evolving. New technologies, research findings, and global partnerships are shaping the future of infectious disease prevention and control.
Investing in research and development is crucial to stay ahead of emerging threats. This includes developing new antibiotics, antiviral drugs, and vaccines, as well as exploring innovative approaches to infection control.
Strengthening public health infrastructure and building capacity in low-resource settings are essential for global health security. Early detection, rapid response, and effective containment are key to mitigating the impact of future outbreaks.
Preparing for the Unexpected: Building Resilience
The COVID-19 pandemic has highlighted the importance of preparedness and resilience in the face of unexpected infectious disease outbreaks.
Building resilient healthcare systems requires investing in surge capacity, developing robust supply chains for essential medical equipment and supplies, and training healthcare workers to respond effectively to outbreaks.
Public health emergency preparedness plans should be regularly reviewed and updated to ensure they are aligned with the latest scientific evidence and best practices. Community engagement and risk communication are essential components of effective emergency preparedness.
The Human Element: Public Awareness and Education
Public awareness and education play a crucial role in preventing and controlling infectious diseases. Educating individuals about infection prevention practices, such as hand hygiene, respiratory etiquette, and vaccination, can significantly reduce the spread of disease.
Empowering individuals to take proactive steps to protect their health is essential for building community resilience. Public health campaigns can provide accurate and timely information about infectious disease risks and promote healthy behaviors.
Clear and concise communication is essential to build trust and encourage public compliance with public health measures. Addressing misinformation and combating rumors are crucial for effective public health communication.
FAQ: Addressing Common Concerns
What are the biggest threats posed by Infection 2025?
The projected trends for Infection 2025 suggest antimicrobial resistance and climate change-driven outbreaks as major threats. These factors could significantly impact global health.
Other potential threats, like urbanization, also contribute to the complexity of the projected landscape for infectious diseases.
Understanding these converging threats is crucial for implementing effective preventive strategies.
How can individuals contribute to mitigating infection outbreaks?
Individuals can play a vital role by practicing good hygiene, staying informed about outbreaks, and supporting public health measures like vaccination.
Responsible antibiotic use is also crucial. By following these recommendations, individuals can contribute to a healthier and more resilient community.
Staying informed about credible sources and avoiding misinformation helps individuals make informed choices regarding their health.
Conclusion
Infection 2025: Projected Outbreak Trends and Data indicates a complex and evolving landscape of infectious diseases. By understanding these trends and investing in proactive measures, we can work towards a healthier and more secure future. So, stay informed, stay prepared, and let’s work together to build a more resilient world. Be sure to check out other informative articles on our site about AI and SEO content related to Infection 2025 and other vital health topics.
Understanding projected outbreak trends and data is crucial for effective mitigation. This knowledge allows for informed decision-making and resource allocation to combat future health crises.
.






