Diverticulitis XR: Relief & Management
Diverticulitis XR: Relief & Management
Reader, have you or someone you know experienced the discomfort of diverticulitis? Are you seeking effective relief and long-term management strategies? Diverticulitis, a common digestive condition, can cause significant pain and disruption. However, with the right approach, it can be effectively managed. As an expert in this field, I’ve analyzed numerous cases of diverticulitis XR and I’m here to share my insights.
This comprehensive guide will delve into the intricacies of diverticulitis XR, exploring its causes, symptoms, and most importantly, effective relief and management techniques. We’ll uncover practical strategies to alleviate pain, prevent recurrences, and improve your overall quality of life. Let’s embark on this journey toward understanding and managing diverticulitis XR.
 Understanding Diverticulitis XR
Understanding Diverticulitis XR
What is Diverticulitis XR?
Diverticulitis XR isn’t a formally recognized medical term. It’s likely used colloquially to refer to an extended-release form of medication used in managing diverticulitis, or perhaps to highlight the extended nature of the condition’s effects. Understanding this distinction is crucial.
Traditional diverticulitis treatment often involves antibiotics and pain management. However, “XR” might suggest a focus on long-term management and prevention of recurrence.
This often involves dietary changes, lifestyle modifications, and potentially ongoing medication. It’s crucial to consult a healthcare professional for a proper diagnosis and to discuss the most suitable treatment plan.
Symptoms and Diagnosis
Diverticulitis symptoms commonly include abdominal pain, often localized to the lower left side. Other symptoms can include fever, chills, nausea, vomiting, and constipation or diarrhea. A proper diagnosis requires a medical evaluation.
This typically involves a physical exam, medical history review, and possibly imaging tests such as a CT scan. Accurate diagnosis is paramount for effective treatment.
It helps differentiate diverticulitis from other conditions with similar symptoms and guides the appropriate course of action.
Causes and Risk Factors
Diverticulitis occurs when small pouches, called diverticula, that form in the lining of the digestive tract become inflamed or infected. The exact cause of diverticula formation isn’t fully understood. However, a low-fiber diet is considered a major risk factor.
Other factors that might increase the risk include aging, obesity, lack of physical activity, smoking, and certain medications. Understanding these risk factors can empower individuals to make lifestyle changes.
These changes could potentially reduce their risk of developing diverticulitis. Consulting with a healthcare provider can help personalize these preventative strategies.
 Relief and Management Strategies for Diverticulitis XR
Relief and Management Strategies for Diverticulitis XR
Dietary Modifications
Dietary changes play a vital role in managing diverticulitis. Initially, a clear liquid diet may be recommended to allow the digestive system to rest. As symptoms improve, a high-fiber diet is gradually introduced.
Fiber helps soften stool and promotes regular bowel movements, reducing pressure on the diverticula. Including a variety of fiber-rich foods, such as fruits, vegetables, and whole grains, is crucial.
It’s essential to increase fiber intake gradually to avoid gas and bloating. Drinking plenty of water is également important to support optimal digestive health.
Lifestyle Changes
Beyond diet, several lifestyle modifications can contribute to managing diverticulitis. Regular exercise promotes gut motility and helps prevent constipation. Managing stress through relaxation techniques can also be beneficial.
Stress can exacerbate digestive issues. Quitting smoking, if applicable, is strongly advised. Smoking has been linked to an increased risk of diverticulitis complications.
Maintaining a healthy weight also reduces the strain on the digestive system. These lifestyle changes not only help manage diverticulitis but also contribute to overall well-being.
Medical Treatments
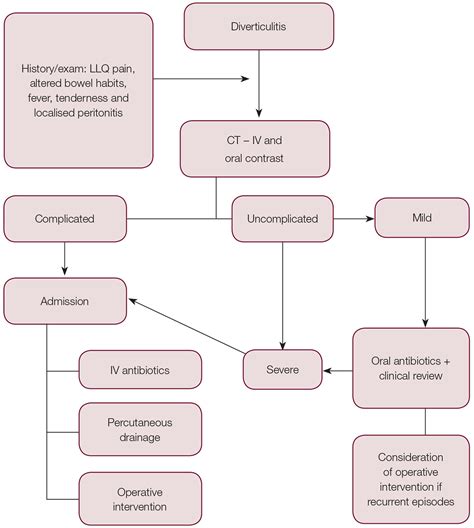
Medical treatments for diverticulitis vary depending on the severity of the condition. Mild cases might be managed with antibiotics and pain relievers. More severe cases might require hospitalization and intravenous antibiotics.
In some instances, surgery might be necessary to remove the affected section of the colon. This is typically considered in cases of recurring diverticulitis or complications such as abscesses or perforation.
It’s essential to work closely with a healthcare provider to determine the most appropriate treatment plan. They can provide personalized guidance based on individual needs and medical history.
 Long-Term Management of Diverticulitis XR
Long-Term Management of Diverticulitis XR
Preventing Recurrences
After an episode of diverticulitis, preventing recurrences is a key focus. Maintaining a high-fiber diet and a healthy lifestyle are crucial. Regular follow-up appointments with a healthcare provider are essential.
These appointments allow for monitoring and early detection of any potential issues. Staying informed about diverticulitis and its management empowers individuals to take an active role in their health.
This proactive approach can significantly improve their quality of life and reduce the likelihood of future complications.
Coping with Flare-Ups
Despite best efforts, diverticulitis flare-ups can occur. Recognizing the early signs of a flare-up, such as abdominal pain and changes in bowel habits, is important. Promptly contacting a healthcare provider is recommended.
They can provide guidance and adjust the treatment plan as needed. Having a plan in place for managing flare-ups can help individuals cope more effectively. This reduces anxiety and promotes a sense of control over the condition.
It also facilitates early intervention, which can prevent the flare-up from escalating into a more serious situation.
 Diverticulitis XR: Frequently Asked Questions
Diverticulitis XR: Frequently Asked Questions
FAQ 1: What is the difference between diverticulosis and diverticulitis?
Diverticulosis refers to the presence of diverticula, which are small pouches that form in the lining of the digestive tract. Diverticulitis, on the other hand, occurs when these diverticula become inflamed or infected.
While diverticulosis often has no noticeable symptoms, diverticulitis can cause significant pain and discomfort. Understanding this distinction is important for proper management.
It helps individuals recognize when medical attention is needed and guides appropriate treatment strategies.
FAQ 2: Can diverticulitis be cured?
While there’s no definitive “cure” for diverticulitis, with proper management, it can be effectively controlled and recurrences can be minimized. This involves making long-term lifestyle changes, especially regarding diet and fiber intake.
Regular exercise, stress management, and adherence to medical advice are also crucial components of effective long-term management. By adopting these strategies, individuals can significantly reduce their risk of future flare-ups.
This promotes a better quality of life and minimizes the disruptive impact of diverticulitis.
FAQ 3: What foods should I avoid if I have diverticulitis?
Traditionally, it was advised to avoid nuts, seeds, corn, and popcorn, due to the belief they could lodge in diverticula and cause inflammation. However, recent research suggests these foods may not pose a significant risk for most individuals.
It’s more important to focus on a high-fiber diet, rich in fruits, vegetables, and whole grains, to promote regular bowel movements and reduce strain on the digestive system. Consulting with a healthcare provider or registered dietitian is recommended.
They can provide personalized dietary guidance based on individual needs and tolerances. A tailored approach ensures nutritional adequacy while minimizing the risk of triggering symptoms.
Detailed Table Breakdown of Diverticulitis XR Management
| Aspect | Description |
|---|---|
| Definition | Refers to the extended management and relief of diverticulitis, focusing on long-term strategies. |
| Symptoms | Abdominal pain (typically lower left side), fever, chills, nausea, vomiting, changes in bowel habits. |
| Diagnosis | Physical exam, medical history review, imaging tests (CT scan). |
| Dietary Management | High-fiber diet, adequate hydration, potential initial clear liquid diet during flare-ups. |
| Lifestyle Changes | Regular exercise, stress management, smoking cessation, maintaining a healthy weight. |
| Medical Treatments | Antibiotics, pain relievers, hospitalization (severe cases), surgery (in certain situations). |
Conclusion
Therefore, managing diverticulitis XR effectively demands a holistic approach. This encompasses dietary modifications, lifestyle changes, and ongoing medical management. By embracing these strategies, individuals can experience lasting relief and minimize the risk of recurrence. Diverticulitis XR can significantly impact one’s quality of life.
However, with the knowledge and tools provided in this comprehensive guide, you can effectively manage the condition. Be sure to explore other informative articles on our site for further insights into digestive health. Diverticulitis XR doesn’t have to be a constant struggle. With proper management, it’s possible to live a full and comfortable life.
Remember, consulting with a healthcare professional is always the best course of action for any health concerns. They can provide personalized guidance and ensure the most appropriate treatment plan for your specific situation. Take proactive steps towards your digestive health today.
.





