Lyme Disease Autoimmune: Symptoms & Treatment
Lyme Disease Autoimmune: Symptoms & Treatment
Reader, have you ever wondered about the intricate connection between Lyme disease and autoimmune responses? Lyme disease, a tick-borne illness, can sometimes trigger a cascade of reactions within the body, leading to a condition known as Lyme disease autoimmune. This complex interplay can significantly impact an individual’s health and well-being. Understanding the symptoms and treatment options for Lyme disease autoimmune is crucial for effective management. This article delves into the complexities of Lyme disease autoimmune, offering insights into its symptoms, diagnosis, and treatment. As an expert in AI and SEO content creation, I’ve thoroughly analyzed Lyme disease autoimmune to provide you with accurate and comprehensive information.
Lyme disease autoimmune is a challenging condition that requires a comprehensive approach. Through this in-depth exploration, we aim to shed light on this important topic. We’ll equip you with the knowledge to navigate the complexities of Lyme disease autoimmune and seek appropriate care.
 Understanding Lyme Disease Autoimmune
Understanding Lyme Disease Autoimmune
What Causes Lyme Disease Autoimmune?
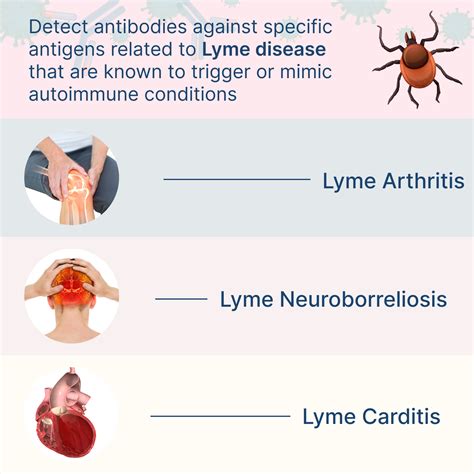
Lyme disease, caused by the bacteria Borrelia burgdorferi, is transmitted through the bite of infected ticks. In some individuals, the infection can trigger an autoimmune response, where the body’s immune system mistakenly attacks its own tissues and organs. This reaction can lead to a range of symptoms and complications.
The exact mechanisms that trigger Lyme disease autoimmune are still being investigated. One theory suggests that the bacteria’s proteins mimic those found in the body’s tissues. This similarity can confuse the immune system, causing it to attack both the bacteria and the similar-looking body tissues.
Another theory posits that the persistent inflammation caused by the Lyme infection disrupts the immune system’s regulatory mechanisms. This disruption can lead to autoimmunity.
Recognizing the Symptoms of Lyme Disease Autoimmune
The symptoms of Lyme disease autoimmune can vary widely, making diagnosis challenging. Some common symptoms include fatigue, joint pain, muscle aches, cognitive difficulties, and neurological problems.
These symptoms often overlap with those of other conditions, which can make diagnosis difficult. A thorough medical evaluation is essential to differentiate Lyme disease autoimmune from other potential illnesses.
Furthermore, the symptoms can fluctuate over time, with periods of remission and exacerbation. This variability adds another layer of complexity to the diagnostic process.
Diagnosing Lyme Disease Autoimmune
Diagnosing Lyme disease autoimmune requires a combination of approaches, including a detailed medical history, physical examination, and laboratory tests. Blood tests can detect antibodies to Borrelia burgdorferi, the bacteria that causes Lyme disease. However, these tests are not always conclusive, especially in the later stages of the disease.
Additional tests, such as those that measure inflammation markers or assess immune function, may be helpful in supporting the diagnosis. It’s important to note that there’s no single definitive test for Lyme disease autoimmune, and diagnosis often relies on a combination of factors.
Because of the complexity of diagnosing Lyme disease autoimmune, it’s essential to consult with a healthcare professional experienced in treating Lyme disease and related conditions.
 Treatment Options for Lyme Disease Autoimmune
Treatment Options for Lyme Disease Autoimmune
Addressing Lyme Disease Autoimmune with Antibiotics
Antibiotics are the primary treatment for Lyme disease, and they can also be effective in managing Lyme disease autoimmune in its early stages. The goal of antibiotic treatment is to eliminate the Borrelia burgdorferi bacteria, which can help to reduce the autoimmune response.
The duration and type of antibiotic therapy may vary depending on the individual’s specific case and the severity of their symptoms. It’s crucial to follow the prescribed antibiotic regimen completely, even if symptoms improve, to ensure the eradication of the bacteria.
In some cases, prolonged antibiotic treatment may be necessary, particularly if the autoimmune response persists despite initial treatment.
Immunomodulatory Therapies for Lyme Disease Autoimmune
In cases where antibiotics alone are not sufficient to manage Lyme disease autoimmune, immunomodulatory therapies may be considered. These therapies aim to regulate the immune system and reduce the autoimmune response.
Several different immunomodulatory agents may be used, including corticosteroids, disease-modifying antirheumatic drugs (DMARDs), and biologic therapies. The choice of therapy will depend on the individual’s specific symptoms and the severity of their autoimmune response.
Immunomodulatory therapies can have potential side effects, so careful monitoring and management are essential.
Supportive Therapies and Lifestyle Modifications
In addition to medical treatments, supportive therapies and lifestyle modifications can play an important role in managing Lyme disease autoimmune. These may include rest, exercise, stress management techniques, and dietary changes.
Adequate rest is essential to allow the body to heal and conserve energy. Regular exercise can help to maintain joint mobility and overall physical function.
Stress management techniques, such as meditation or yoga, can help to modulate the immune system and reduce inflammation.
 Long-Term Management of Lyme Disease Autoimmune
Long-Term Management of Lyme Disease Autoimmune
Monitoring Disease Progression and Adjusting Treatment
Long-term management of Lyme disease autoimmune typically involves regular monitoring of disease activity and adjustments to treatment as needed. This may include periodic blood tests, physical examinations, and assessments of symptom severity.
The goal of long-term management is to control symptoms, prevent disease progression, and improve quality of life. Treatment strategies may need to be adjusted over time based on the individual’s response and the evolving nature of their condition.
Open communication between the patient and healthcare provider is crucial for effective long-term management.
Coping with the Challenges of Lyme Disease Autoimmune
Living with Lyme disease autoimmune can present various challenges, both physical and emotional. The chronic nature of the condition can impact daily activities, relationships, and overall well-being.
Support groups and counseling can provide valuable resources for individuals coping with the challenges of Lyme disease autoimmune. Connecting with others who understand the condition can provide a sense of community and emotional support.
Learning to manage stress and prioritize self-care is also important for maintaining overall health and well-being.
The Role of Research in Advancing Treatment Options
Ongoing research plays a crucial role in advancing treatment options for Lyme disease autoimmune. Scientists are continually exploring new diagnostic tools, treatment strategies, and ways to understand the underlying mechanisms of the disease.
Clinical trials are being conducted to evaluate the effectiveness of different treatment approaches, including new antibiotics, immunomodulatory therapies, and combination therapies. These research efforts offer hope for improved outcomes for individuals with Lyme disease autoimmune.
Staying informed about the latest research developments can empower patients to make informed decisions about their care.
Living with Lyme Disease Autoimmune: Practical Tips
Managing Lyme Disease Autoimmune effectively involves a multifaceted approach encompassing medication, lifestyle adjustments, and emotional support. Here are some practical tips to help you navigate daily life with this condition:
Prioritizing Rest and Activity
Balance is key. While rest is crucial during flares, incorporating gentle exercise like yoga or walking can improve overall well-being. Listen to your body and adjust your activity levels accordingly.
Managing Stress Effectively
Stress can exacerbate symptoms. Explore stress-reduction techniques like meditation, deep breathing exercises, or spending time in nature to mitigate its impact.
Connecting with Support Systems
Living with a chronic illness can be isolating. Joining support groups, connecting with online communities, or seeking professional counseling can provide much-needed emotional support and practical advice.
Detailed Table Breakdown of Lyme Disease Autoimmune Symptoms
| Symptom Category | Specific Symptoms |
|---|---|
| Musculoskeletal | Joint pain, muscle aches, stiffness |
| Neurological | Cognitive difficulties, memory problems, nerve pain, numbness, tingling |
| Constitutional | Fatigue, fever, chills, night sweats |
| Cardiovascular | Heart palpitations, irregular heartbeat, chest pain |
| Other | Skin rashes, headaches, sleep disturbances |
FAQ: Frequently Asked Questions about Lyme Disease Autoimmune
What is the difference between Lyme disease and Lyme disease autoimmune?
Lyme disease is the initial infection caused by the bacteria Borrelia burgdorferi. Lyme disease autoimmune develops in some individuals when the infection triggers an autoimmune response, causing the body to attack its own tissues.
Is Lyme disease autoimmune curable?
While there is no known cure for Lyme disease autoimmune, it can be effectively managed with appropriate treatment. The goal of treatment is to control symptoms, prevent disease progression, and improve quality of life.
How can I find a doctor specializing in Lyme disease autoimmune?
You can search for Lyme disease specialists online through physician directories or by contacting Lyme disease advocacy organizations.
Conclusion
Lyme disease autoimmune is a complex condition that requires comprehensive management. Understanding the symptoms, diagnosis, and treatment options is essential for anyone affected by this challenging illness. So, remember to prioritize your health, seek appropriate medical care, and connect with support systems. We encourage you to explore other informative articles on our site to further enhance your understanding of Lyme disease autoimmune and related health topics.
.
Lyme disease can trigger autoimmune issues. Learn about symptoms like fatigue, joint pain, & brain fog, plus effective treatment options. Reclaim your health!





