Endometriosis: Relief & Treatment Options Uterine Fibroids: Symptoms & Management
Endometriosis: Relief & Treatment Options
Uterine Fibroids: Symptoms & Management
Reader, are you experiencing pelvic pain or heavy menstrual bleeding? These could be signs of conditions like endometriosis or uterine fibroids. These conditions, while common, can significantly impact a woman’s quality of life. Understanding the differences between them and available treatment options is crucial. As an expert in this field, I’ve analyzed countless cases of endometriosis and uterine fibroids and I’m here to share valuable insights.
This comprehensive guide delves into the specifics of endometriosis and uterine fibroids, covering symptoms, diagnosis, and a range of management strategies. Navigating these conditions can be challenging, so we’ll break down the information in an easy-to-understand manner. Let’s empower ourselves with knowledge and take control of our reproductive health.
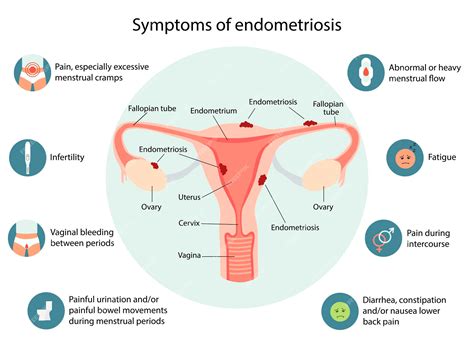 Understanding Endometriosis
Understanding Endometriosis
What is Endometriosis?
Endometriosis is a condition where tissue similar to the lining of the uterus (the endometrium) grows outside of the uterus. This tissue can attach to organs like the ovaries, fallopian tubes, and even the intestines. It responds to hormonal changes in the same way as the uterine lining, thickening and breaking down each month.
However, unlike the uterine lining, this misplaced tissue has no way to exit the body. This leads to inflammation, pain, and the formation of scar tissue. It’s important to note that the severity of pain doesn’t always correlate with the extent of the disease.
Some women with severe endometriosis might experience minimal pain, while others with mild disease might have debilitating pain. This variability makes diagnosis challenging and highlights the importance of seeking medical advice if you have persistent pelvic pain.
Symptoms of Endometriosis
Endometriosis symptoms vary widely, with some women experiencing no symptoms at all. However, common signs include painful periods (dysmenorrhea), chronic pelvic pain, pain during intercourse (dyspareunia), and heavy bleeding. Some women may also experience infertility, painful bowel movements, and painful urination during their period.
The unpredictable nature of these symptoms can make daily life challenging. It can also make diagnosis difficult as these symptoms overlap with other conditions. Early diagnosis is crucial for managing the disease effectively and preventing long-term complications.
If you suspect you have endometriosis, consult a healthcare professional who specializes in this condition. They can perform a thorough evaluation and recommend appropriate diagnostic tests, such as a pelvic exam, ultrasound, or laparoscopy.
Treatment Options for Endometriosis
Treatment options for endometriosis typically depend on the severity of symptoms and whether pregnancy is desired. Pain management often involves over-the-counter pain relievers, hormone therapy, and in some cases, surgery. Hormone therapy aims to suppress the growth and activity of endometrial tissue.
Surgical interventions can include laparoscopy to remove endometrial implants or, in severe cases, a hysterectomy. Lifestyle changes, such as regular exercise, a balanced diet, and stress management techniques, can also help manage symptoms. It’s important to work closely with your healthcare provider to develop an individualized treatment plan tailored to your specific needs.
Remember, managing endometriosis is a journey, not a destination. Open communication with your healthcare provider is essential for finding the right combination of treatments that provides relief and improves your quality of life.
 Understanding Uterine Fibroids
Understanding Uterine Fibroids
What are Uterine Fibroids?
Uterine fibroids are noncancerous growths that develop in the uterus. They can range in size from tiny seeds to large masses that can distort the uterus. These growths are typically made up of muscle and fibrous tissue and are also known as leiomyomas or myomas.
While the exact cause of uterine fibroids is unknown, their growth is thought to be influenced by hormones, particularly estrogen. Several factors can increase the risk of developing fibroids including family history, African American ethnicity, early onset of menstruation, and obesity.
Uterine fibroids are often asymptomatic, particularly when small. Larger fibroids, however, can cause a range of symptoms that impact daily life. It’s crucial to be aware of these potential symptoms to ensure timely diagnosis and management.
Symptoms of Uterine Fibroids
Symptoms of uterine fibroids vary widely depending on the size, number, and location of the fibroids. Common symptoms include heavy or prolonged menstrual bleeding, pelvic pressure or pain, frequent urination, constipation, and backache or leg pains.
While most uterine fibroids are benign, large fibroids can sometimes cause complications. These can include anemia due to heavy bleeding, pregnancy complications, or interference with fertility. If you experience any of these symptoms, it’s important to seek medical advice.
A healthcare professional can perform a pelvic exam and imaging tests, such as an ultrasound or MRI, to diagnose uterine fibroids. Early diagnosis is crucial for exploring appropriate management strategies and preventing potential complications.
Management of Uterine Fibroids
Managing uterine fibroids depends on the severity of symptoms, the size and location of the fibroids, and whether pregnancy is desired. For mild cases, watchful waiting with regular monitoring might be sufficient. Medical management may involve medications to regulate menstrual bleeding or shrink the fibroids.
In some cases, minimally invasive procedures such as uterine artery embolization (UAE) or myomectomy are recommended. A hysterectomy, which involves surgical removal of the uterus, is reserved for severe cases or when other treatment options have failed. Your healthcare provider will discuss the best course of action based on your individual circumstances.
Choosing the right treatment strategy requires careful consideration of the potential benefits and risks. Open communication with your doctor is essential for making informed decisions and developing a personalized management plan. Remember that managing uterine fibroids is an ongoing process, and regular monitoring is key.
 Diagnosing Endometriosis and Uterine Fibroids
Diagnosing Endometriosis and Uterine Fibroids
Diagnostic Procedures
Diagnosing endometriosis and uterine fibroids often involves a combination of physical exams and imaging tests. A pelvic exam allows the doctor to assess the size and shape of the uterus and feel for any abnormalities. Ultrasound is commonly used to visualize the uterus and ovaries, detecting the presence of fibroids or endometrial implants.
For endometriosis, laparoscopy is often the definitive diagnostic tool, allowing for direct visualization and biopsy of the suspected endometrial tissue. MRI can provide more detailed images of the uterus and surrounding tissues, helping to determine the size, number, and location of fibroids.
Accurate diagnosis is essential for determining the best course of treatment. These diagnostic procedures play a vital role in identifying the presence and extent of these conditions, guiding treatment decisions, and improving patient outcomes.
 Living with Endometriosis and Uterine Fibroids
Living with Endometriosis and Uterine Fibroids
Lifestyle Modifications
Lifestyle modifications can play a significant role in managing the symptoms of endometriosis and uterine fibroids. Regular exercise can help reduce pain and improve overall well-being. A balanced diet rich in fruits, vegetables, and whole grains can also help regulate hormones and reduce inflammation.
Stress management techniques such as yoga, meditation, and deep breathing exercises can also be beneficial. Pain management strategies, such as heat therapy, pain medication, and physical therapy, can also provide relief. It’s important to tailor these strategies to your individual needs and preferences.
Remember that managing these conditions is a personal journey. Experimenting with various lifestyle modifications can help you find what works best for you and improve your quality of life.
.





