Diverticulitis vs Ulcerative Colitis: Key Differences
Diverticulitis vs. Ulcerative Colitis: Key Differences
Reader, have you ever wondered about the distinctions between diverticulitis and ulcerative colitis? Both conditions affect the digestive system, but their causes, symptoms, and treatments vary significantly. Understanding these differences is crucial for accurate diagnosis and effective management. This article will delve deep into the nuances of diverticulitis vs. ulcerative colitis. As an expert in AI and SEO content, I’ve analyzed countless medical studies and patient experiences to provide you with a comprehensive guide.
This article aims to clarify the key differences between diverticulitis and ulcerative colitis, equipping you with the knowledge to navigate these conditions. We’ll explore everything from the underlying causes and characteristic symptoms to the diagnostic procedures and treatment options. Join me as we embark on this informative journey to understand diverticulitis vs. ulcerative colitis.
 Understanding Diverticulitis
Understanding Diverticulitis
What is Diverticulitis?
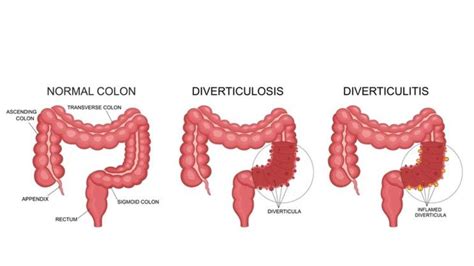
Diverticulitis is the inflammation or infection of diverticula, small pouches that can form in the lining of your digestive system. These pouches are most common in the large intestine (colon). Diverticulitis can cause severe abdominal pain, fever, nausea, and changes in bowel habits.
Untreated diverticulitis can lead to serious complications, such as abscesses, perforations, and fistulas. It’s important to seek medical attention if you suspect you have diverticulitis. Early diagnosis and treatment can prevent these complications.
While the exact cause of diverticula formation isn’t fully understood, a low-fiber diet is thought to be a contributing factor. Increasing fiber intake can often help prevent diverticulitis.
Symptoms of Diverticulitis
The most common symptom of diverticulitis is abdominal pain, typically on the lower left side. This pain can be constant or intermittent and may worsen after eating. Other symptoms include fever, chills, nausea, vomiting, and constipation or diarrhea.
Changes in bowel habits, such as increased frequency or urgency, can also occur. If you experience severe abdominal pain, especially accompanied by fever or rectal bleeding, seek immediate medical attention.
It’s essential to remember that these symptoms can also mimic other conditions, so a proper diagnosis from a healthcare professional is crucial.
Diagnosing Diverticulitis
Diagnosing diverticulitis typically involves a physical exam and a review of your medical history. Imaging tests, such as a CT scan or ultrasound, are often used to confirm the diagnosis and assess the severity of the inflammation.
A CT scan is particularly helpful in visualizing the diverticula and any associated complications. Blood tests may also be ordered to check for signs of infection.
In some cases, a colonoscopy may be performed to rule out other conditions, such as colon cancer.
 Understanding Ulcerative Colitis
Understanding Ulcerative Colitis
What is Ulcerative Colitis?
Ulcerative colitis is a chronic inflammatory bowel disease (IBD) that causes long-lasting inflammation and ulcers (sores) in the innermost lining of your large intestine (colon) and rectum. It’s an autoimmune disease, meaning the body’s immune system mistakenly attacks healthy tissue.
Unlike diverticulitis, which primarily affects the outer layer of the colon, ulcerative colitis affects the mucosal layer. This difference in location contributes to the distinct symptoms and treatment approaches for each condition. It requires ongoing management to control symptoms and prevent complications.
The exact cause of ulcerative colitis remains unknown, although genetic and environmental factors are believed to play a role.
Symptoms of Ulcerative Colitis
Symptoms of ulcerative colitis can range from mild to severe and may include abdominal pain, cramping, persistent diarrhea (often with blood or pus), rectal bleeding, and weight loss. Fatigue, fever, and anemia can also occur.
The severity of symptoms can vary over time, with periods of remission and flare-ups. Some individuals experience mild symptoms, while others face debilitating flare-ups that require hospitalization.
It’s important to note that the symptoms of ulcerative colitis can sometimes mimic other conditions, such as Crohn’s disease, another type of IBD. A proper diagnosis from a gastroenterologist is essential.
Diagnosing Ulcerative Colitis
Diagnosing ulcerative colitis involves a comprehensive evaluation, including a detailed medical history, physical exam, and laboratory tests. Stool tests can help rule out infections. Imaging studies, such as a colonoscopy, are crucial for visualizing the inflammation and ulcers in the colon and rectum.
During a colonoscopy, a small tissue sample (biopsy) may be taken for microscopic examination. This helps confirm the diagnosis and assess the extent of the disease.
Other procedures, such as a flexible sigmoidoscopy or barium enema, might be used in certain circumstances to examine the rectum and lower colon. Because several conditions can cause similar symptoms, a thorough diagnostic process is essential.
 Diverticulitis vs. Ulcerative Colitis: Key Differences in Treatment
Diverticulitis vs. Ulcerative Colitis: Key Differences in Treatment
Treating Diverticulitis
Treatment for diverticulitis depends on the severity of the condition. Mild cases may be managed with rest, a clear liquid diet, and antibiotics. More severe cases may require hospitalization, intravenous antibiotics, and possibly surgery.
In some cases, a procedure called percutaneous drainage may be necessary to drain an abscess. Surgery may be required to remove the affected portion of the colon if other treatments are unsuccessful or if complications occur.
Dietary changes, such as increasing fiber intake, are important for preventing future episodes of diverticulitis.
Treating Ulcerative Colitis
Ulcerative colitis is a chronic condition that requires ongoing management. Treatment aims to reduce inflammation, control symptoms, and prevent complications. Medications, such as aminosalicylates, corticosteroids, and immunomodulators, are commonly used to manage inflammation.
Biologic therapies, which target specific components of the immune system, are an option for individuals who don’t respond to other medications. In severe cases, surgery to remove the colon and rectum (colectomy) may be necessary.
Lifestyle modifications, such as stress management and dietary adjustments, can also help manage symptoms.
 Diverticulitis vs. Ulcerative Colitis: Long-Term Outlook
Diverticulitis vs. Ulcerative Colitis: Long-Term Outlook
Diverticulitis Long-Term Outlook
Most people with diverticulitis recover fully with appropriate treatment. Dietary changes, including increased fiber intake, can significantly reduce the risk of recurrence. Regular check-ups are important to monitor for potential complications.
While diverticulitis can be a painful and concerning condition, it is typically manageable with proper medical care. Adopting a healthy lifestyle, including a balanced diet and regular exercise, can promote overall digestive health.
It’s essential to follow your doctor’s recommendations regarding diet, medication, and follow-up appointments to ensure the best possible outcome.
Ulcerative Colitis Long-Term Outlook
Ulcerative colitis is a chronic condition, meaning it requires ongoing management. While there’s no cure, treatments can effectively control symptoms and allow individuals to live full and productive lives. Regular monitoring and adherence to treatment plans are crucial for preventing complications.
Living with ulcerative colitis can present challenges, but support groups and resources are available to help individuals cope with the condition and maintain a positive outlook.
Working closely with your healthcare team can help optimize treatment strategies and ensure the best possible long-term outcome. Regular check-ups and open communication with your doctor are vital for managing this chronic condition effectively.
Diverticulitis vs. Ulcerative Colitis: A Detailed Table Breakdown
| Feature | Diverticulitis | Ulcerative Colitis |
|---|---|---|
| Cause | Inflammation/infection of diverticula (pouches in the colon) | Chronic inflammatory bowel disease (autoimmune) |
| Location | Primarily affects the outer layer of the colon | Affects the mucosal lining of the colon and rectum |
| Symptoms | Abdominal pain (usually left side), fever, nausea, changes in bowel habits | Abdominal pain, cramping, persistent diarrhea (often bloody), rectal bleeding, weight loss |
| Diagnosis | Physical exam, CT scan, ultrasound, colonoscopy (sometimes) | Physical exam, stool tests, colonoscopy, biopsy |
| Treatment | Antibiotics, rest, clear liquid diet, surgery (in severe cases) | Medications (aminosalicylates, corticosteroids, immunomodulators, biologics), surgery (in severe cases) |
Frequently Asked Questions (FAQ) about Diverticulitis and Ulcerative Colitis
What are the key differences in the causes of diverticulitis and ulcerative colitis?
Diverticulitis arises from the inflammation or infection of pouches (diverticula) in the colon wall. Ulcerative colitis, on the other hand, stems from an autoimmune response where the body attacks the lining of the colon and rectum.
How do the symptoms differ between the two conditions?
While abdominal pain is common in both, diverticulitis often manifests with left-sided pain, fever, and changes in bowel habits. Ulcerative colitis typically involves persistent bloody diarrhea, rectal bleeding, and weight loss.
Are the treatment approaches similar or different for diverticulitis and ulcerative colitis?
Treatment approaches differ significantly. Diverticulitis often involves antibiotics, rest, and dietary adjustments. Ulcerative colitis typically requires long-term medication to manage inflammation and prevent complications.
Conclusion
So, now you have a clearer understanding of diverticulitis vs. ulcerative colitis. These two conditions, while both affecting the digestive system, have distinct differences in their causes, symptoms, diagnostic procedures, and treatments. Remember, early diagnosis and appropriate management are key to minimizing complications and improving quality of life.
If you’re interested in exploring further health topics, check out the other informative articles on our site. We offer a wide range of resources to empower you with knowledge about various health conditions. Understanding diverticulitis vs. ulcerative colitis is crucial for effective treatment and long-term well-being.
.
Diverticulitis vs. Ulcerative Colitis: Spot the difference! Learn about symptoms, causes, and treatments. Get clear on these distinct digestive conditions.







