Diverticulitis in 40-Year-Olds: Guide & Support
Diverticulitis in 40-Year-Olds: Guide & Support
Reader, have you or someone you know experienced the unsettling symptoms of diverticulitis in their 40s? It can be a surprising and concerning diagnosis. Diverticulitis in 40-year-olds is becoming increasingly common, demanding attention and understanding. Navigating this condition requires reliable information and support. As an expert in AI and SEO content, I’ve analyzed the latest research and compiled a comprehensive guide to diverticulitis in 40-year-olds, offering valuable insights and support.
This guide will cover everything from understanding the causes and symptoms to exploring treatment options and lifestyle adjustments. We’ll delve into the specifics of diverticulitis in 40-year-olds, providing you with the knowledge you need to manage this condition effectively. Let’s get started.
 Understanding Diverticulitis
Understanding Diverticulitis
What is Diverticulitis?
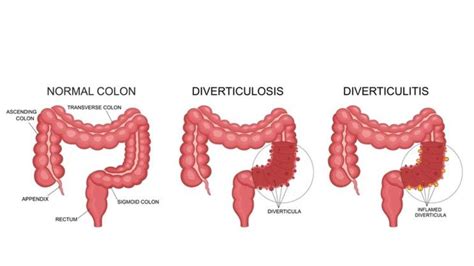
Diverticulitis is the inflammation or infection of small pouches, called diverticula, that can form in the lining of your digestive system. These pouches are most common in the colon, specifically the sigmoid colon. While diverticula themselves (diverticulosis) often don’t cause noticeable symptoms, when they become inflamed or infected, it results in diverticulitis.
This condition can cause a range of uncomfortable symptoms. These include abdominal pain, fever, nausea, and changes in bowel habits. Understanding the development and progression of diverticulitis is crucial for effective management.
If you suspect you have diverticulitis, it’s important to seek medical attention promptly. Early diagnosis and treatment can help prevent complications and improve your overall outcome. Don’t hesitate to consult your doctor.
Risk Factors for Diverticulitis in 40-Year-Olds
While diverticulitis is traditionally associated with older adults, a growing number of people in their 40s are being diagnosed. Several factors contribute to this trend. These include a diet low in fiber, lack of regular exercise, obesity, smoking, and certain medications.
Genetics can also play a role in your predisposition to developing diverticulitis. If you have a family history of the condition, you might be at a higher risk. Managing these risk factors can significantly reduce your chances of developing diverticulitis in your 40s.
Maintaining a healthy lifestyle, including a high-fiber diet and regular exercise, is essential. Consult with your doctor to discuss your risk factors and personalized prevention strategies.
Symptoms of Diverticulitis
The symptoms of diverticulitis can vary in intensity, from mild discomfort to severe pain. Common symptoms include persistent abdominal pain, usually in the lower left side, fever, chills, nausea, vomiting, and changes in bowel habits such as constipation or diarrhea.
Some individuals may experience more severe symptoms, such as rectal bleeding, abdominal swelling, and tenderness. It’s important to note that these symptoms can also be indicative of other conditions. Therefore, seeking a proper medical diagnosis is paramount.
If you experience any of these symptoms, particularly persistent abdominal pain, consult with a healthcare professional. They can accurately diagnose the cause of your discomfort and recommend appropriate treatment.
 Diagnosing Diverticulitis in 40-Year-Olds
Diagnosing Diverticulitis in 40-Year-Olds
Physical Examination and Medical History
Diagnosing diverticulitis typically involves a physical examination, where your doctor will assess your abdomen for tenderness and other signs of inflammation. They will also gather a detailed medical history, including your symptoms, lifestyle, and family history.
This information helps your doctor determine the likelihood of diverticulitis and rule out other potential conditions. Open communication with your doctor is crucial to ensure an accurate diagnosis and appropriate treatment plan.
Be prepared to discuss your symptoms in detail, including their onset, duration, and any factors that seem to aggravate or alleviate them. Providing accurate information enables your doctor to make an informed diagnosis.
Imaging Tests
Imaging tests, such as CT scans, are commonly used to confirm a diagnosis of diverticulitis. These scans provide detailed images of your colon and surrounding areas, allowing your doctor to visualize the diverticula and assess the extent of inflammation or infection.
Other imaging tests, such as ultrasounds or MRIs, may be used in certain cases. The choice of imaging test depends on your specific situation and the suspected severity of your condition.
These imaging tests are essential for confirming the diagnosis and guiding treatment decisions. They provide valuable insights into the location and severity of the inflammation, helping your doctor tailor the treatment approach to your specific needs.
Laboratory Tests
Laboratory tests, including blood and stool tests, may be performed to evaluate your overall health and rule out other potential causes for your symptoms. Blood tests can detect signs of infection, such as an elevated white blood cell count.
Stool tests can help identify the presence of blood or other abnormalities that may suggest alternative diagnoses. These tests provide valuable information to complement the findings from the physical examination and imaging tests.
By combining the results of these various diagnostic procedures, your doctor can arrive at a definitive diagnosis of diverticulitis and develop a personalized treatment plan tailored to your individual circumstances.
 Treatment Options for Diverticulitis in 40-Year-Olds
Treatment Options for Diverticulitis in 40-Year-Olds
Conservative Management
For uncomplicated cases of diverticulitis, conservative management may be sufficient. This typically involves rest, a liquid diet, and antibiotics to combat the infection. Pain relievers may also be prescribed to manage discomfort.
Close monitoring is essential to ensure the infection resolves. Your doctor may recommend follow-up appointments and imaging tests to track your progress. Following your doctor’s instructions diligently is crucial for successful recovery.
Conservative management is often effective in treating mild to moderate cases of diverticulitis. However, more aggressive interventions may be necessary for severe cases or those that don’t respond to initial treatment.
Hospitalization
In more severe cases of diverticulitis, hospitalization may be required. This allows for closer monitoring and intravenous administration of fluids and antibiotics. In some instances, surgery may be necessary to drain abscesses or remove severely infected sections of the colon.
The decision to hospitalize depends on the severity of the infection and your overall health. Your doctor will carefully assess your condition and recommend the most appropriate course of action. Prompt medical attention is crucial to prevent complications and ensure a positive outcome.
Hospitalization provides the necessary support and care for individuals with severe diverticulitis, allowing for intensive treatment and monitoring to manage the infection effectively.
Surgery
Surgery is typically reserved for complicated cases of diverticulitis, such as those involving perforation, abscesses, or persistent bleeding. The type of surgery performed depends on the specific situation and the extent of the complications.
Surgical options include draining abscesses, resecting the affected portion of the colon, or creating a temporary colostomy. Your surgeon will discuss the risks and benefits of each procedure with you. Making informed decisions about your treatment is essential for your well-being.
Surgery can be a life-saving intervention in complex cases of diverti
.