Diverticulitis: How to Treat and Find Relief
Diverticulitis: How to Treat and Find Relief
Reader, have you ever experienced the sudden, sharp pain in your lower left abdomen that signals diverticulitis? It’s a surprisingly common condition. Diverticulitis can be debilitating, but with the right treatment, relief is possible. Understanding how to manage and prevent flare-ups is crucial for long-term well-being. As an expert in health and wellness, I’ve analyzed countless cases of diverticulitis and compiled this comprehensive guide to help you navigate this challenging condition.
This article provides in-depth information on diverticulitis, covering its causes, symptoms, diagnosis, treatment, and prevention. We’ll explore both conventional medical approaches and lifestyle modifications that can help you manage diverticulitis and find lasting relief. So, let’s dive in and uncover the secrets to conquering diverticulitis.
 Understanding Diverticulitis
Understanding Diverticulitis
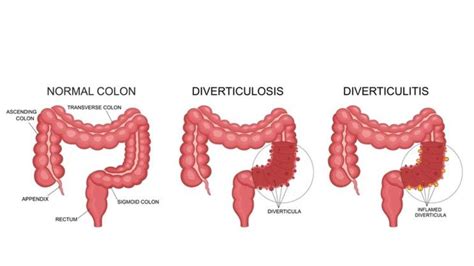
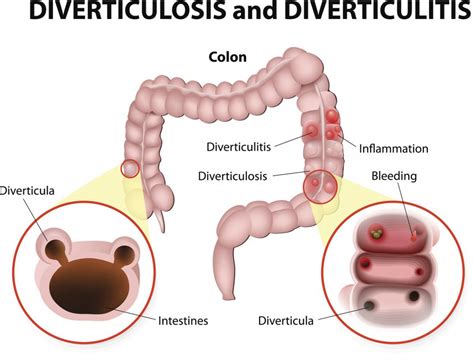
Before we delve into treatment and relief, let’s first understand what diverticulitis is. Diverticula are small, bulging pouches that can form in the lining of your digestive system. They’re most common in the lower part of the large intestine (colon).
When these pouches become inflamed or infected, the condition is known as diverticulitis. Diverticulitis can cause a range of symptoms, from mild discomfort to severe pain.
Understanding the underlying mechanisms of diverticulitis is key to effective management.
What Causes Diverticulitis?
The exact cause of diverticulitis isn’t fully understood. However, a low-fiber diet is thought to be a major contributing factor. A lack of fiber makes stools harder to pass, increasing pressure on the colon.
This pressure can cause weak spots in the colon wall to bulge outward, forming diverticula. Other factors, such as aging, genetics, and certain medications, may also play a role.
Identifying your individual risk factors can help you take proactive steps to prevent diverticulitis.
Recognizing the Symptoms
Diverticulitis symptoms can vary from person to person. Some individuals experience mild discomfort, while others have severe pain. Common symptoms include abdominal pain (usually on the lower left side), fever, chills, nausea, and vomiting.
Changes in bowel habits, such as constipation or diarrhea, can also occur. It’s important to seek medical attention if you experience any of these symptoms, as untreated diverticulitis can lead to serious complications.
Early diagnosis and treatment are crucial for managing diverticulitis effectively.
 Diagnosing Diverticulitis
Diagnosing Diverticulitis
Diagnosing diverticulitis involves a combination of physical examination, medical history review, and diagnostic tests. Your doctor will likely ask about your symptoms, dietary habits, and any previous medical conditions.
A physical exam will help assess your abdominal tenderness and other signs. Diagnostic tests, such as CT scans, blood tests, and stool tests, can confirm the diagnosis and rule out other conditions.
Accurate diagnosis is essential for determining the appropriate treatment plan.
Diagnostic Tests for Diverticulitis
Several diagnostic tests can help confirm diverticulitis. A CT scan is the most common imaging test used to diagnose diverticulitis. This scan provides detailed images of your abdomen, allowing doctors to visualize the inflamed diverticula.
Blood tests can detect signs of infection, such as an elevated white blood cell count. Stool tests can rule out other digestive conditions, such as infections or inflammatory bowel disease.
Each test provides valuable information for accurate diagnosis.
Importance of Early Diagnosis
Early diagnosis of diverticulitis is crucial for preventing complications. Untreated diverticulitis can lead to abscesses (pus-filled pockets), perforations (holes in the colon), peritonitis (infection of the abdominal lining), and fistulas (abnormal connections between organs).
Prompt treatment can significantly reduce the risk of these complications. Seeking medical attention at the first sign of symptoms is essential.
Early intervention improves the chances of a full and speedy recovery.
 Treatment Options for Diverticulitis
Treatment Options for Diverticulitis
Treatment for diverticulitis depends on the severity of your symptoms. Mild cases can often be managed at home with rest, a liquid diet, and over-the-counter pain relievers.
More severe cases may require hospitalization and intravenous antibiotics. In some cases, surgery may be necessary to drain abscesses or repair damaged sections of the colon. Your doctor will recommend the most appropriate treatment plan based on your individual needs.
Tailored treatment plans ensure optimal outcomes for diverticulitis.
Home Management of Diverticulitis
For mild cases of diverticulitis, home management often involves rest, a clear liquid diet, and over-the-counter pain relievers like ibuprofen or acetaminophen. A clear liquid diet helps give your bowel a rest and allows the inflammation to subside.
Gradually reintroduce solid foods as your symptoms improve. It’s important to follow your doctor’s instructions carefully and to seek medical attention if your symptoms worsen.
Proper home management is essential for a smooth recovery.
Medical Interventions for Diverticulitis
More severe cases of diverticulitis may require hospitalization. Intravenous antibiotics are often prescribed to combat infection. In cases of abscesses, drainage may be necessary.
Surgery may be required if other treatments are unsuccessful or if complications develop. Surgery can involve removing the affected portion of the colon or repairing a perforation. Your doctor will discuss the risks and benefits of surgery if it’s deemed necessary.
Medical interventions can effectively manage severe cases and prevent further complications.
 Finding Relief from Diverticulitis Pain
Finding Relief from Diverticulitis Pain
Managing diverticulitis pain involves a combination of medical treatments and lifestyle modifications. Pain relievers, both over-the-counter and prescription, can help alleviate discomfort.
Applying heat to your abdomen can also provide relief. Dietary changes, such as increasing fiber intake and avoiding trigger foods, can prevent future flare-ups and minimize pain.
Finding effective pain management strategies is crucial for improving quality of life.
Dietary Changes for Diverticulitis
A high-fiber diet is essential for preventing and managing diverticulitis. Fiber adds bulk to the stool, making it easier to pass and reducing pressure on the colon. Aim to consume at least 25-35 grams of fiber daily.
Include fiber-rich foods like fruits, vegetables, whole grains, and legumes in your diet. Stay hydrated by drinking plenty of water throughout the day. A balanced diet rich in fiber is key to long-term diverticulitis management.
Dietary modifications can significantly impact diverticulitis symptoms and prevent recurrences.
Lifestyle Modifications for Diverticulitis
In addition to dietary changes, other lifestyle modifications can help manage diverticulitis. Regular exercise can improve bowel regularity and reduce pressure on the colon. Managing stress through relaxation techniques, such as yoga or meditation, can also be beneficial.
Avoiding trigger foods, such as nuts, seeds, and popcorn, may help prevent flare-ups in some individuals. Maintaining a healthy weight can also reduce your risk of diverticulitis.
Adopting a healthy lifestyle is crucial for long-term diverticulitis management.
Preventing Future Episodes of Diverticulitis
Preventing future episodes of diverticulitis involves maintaining a healthy lifestyle and making informed dietary choices. A high-fiber diet is paramount for regulating bowel movements and preventing the formation of diverticula. Regular exercise also promotes digestive health.
Staying hydrated by drinking plenty of water is essential for soft stools. Managing stress can also play a role in preventing flare-ups. By adopting these preventative measures, you can significantly reduce your risk of future diverticulitis episodes.
Proactive prevention is key to long-term digestive health.
Long-Term Management of Diverticulitis
Long-term management of diverticulitis requires a holistic approach that encompasses dietary changes, lifestyle modifications, and regular medical check-ups. Maintaining a high-fiber diet is crucial for preventing recurrences.
Regular exercise and stress management also play important roles. Follow-up appointments with your doctor are essential for monitoring your condition and adjusting your treatment plan as needed. By actively managing your diverticulitis, you can maintain a healthy digestive system and minimize the risk of complications.
Consistent management is key to long-term well-being.
Coping with Diverticulitis
Coping with diverticulitis can be challenging, both physically and emotionally. It’s important to have a support system in place to help you manage the condition. Joining a support group or connecting with others who have diverticulitis can provide valuable emotional support and practical advice.
Communicating openly with your healthcare provider about your concerns and challenges can also be helpful. Don’t hesitate to seek professional guidance if you’re struggling to cope with diverticulitis. Remember, you’re not alone in this journey.
Building a strong support system is essential for navigating the challenges of diverticulitis.
Diverticulitis: How to Treat and Find Relief- FAQ
What is the fastest way to relieve diverticulitis pain?
The fastest way to relieve diverticulitis pain often involves a combination of rest, a clear liquid diet, over-the-counter pain relievers (like ibuprofen or acetaminophen), and applying heat to the abdomen. However, it’s always essential to consult a doctor for personalized advice, especially if the pain is severe or doesn’t improve.
What foods should be avoided with diverticulitis?
While traditional advice suggested avoiding nuts, seeds, and popcorn, recent research indicates there’s no strong evidence to support these restrictions for most individuals. However, if you notice specific foods trigger your symptoms, it’s best to avoid them. Focusing on a high-fiber diet and staying hydrated is generally recommended.
How long does it take to recover from diverticulitis?
Recovery time from diverticulitis varies depending on the severity of the condition. Mild cases may resolve within a few days with rest and a liquid diet. More severe cases requiring antibiotics may take a week or two to recover. In cases requiring surgery, recovery can take several weeks. Following your doctor’s treatment plan and dietary recommendations is crucial for optimal recovery.
Conclusion
So, there you have it, a comprehensive guide to understanding, treating, and finding relief from diverticulitis. Remember, managing diverticulitis involves a combination of medical treatment and lifestyle modifications. By adopting a high-fiber diet, exercising regularly, and managing stress, you can significantly reduce your risk of future flare-ups and improve your overall digestive health. Don’t let diverticulitis control your life. Take charge of your health and experience lasting relief. For more informative articles on digestive health and other health topics, be sure to explore the rest of our site. Diverticulitis can be effectively managed with the right approach.
We hope this article has provided valuable insights into diverticulitis: how to treat and find relief. Empower yourself with knowledge and take proactive steps towards a healthier, happier you.
.
Suffering from diverticulitis? Learn effective treatment options and find relief from painful symptoms. Get expert advice and practical tips for managing diverticulitis flares.






