Diverticulitis Infection: Symptoms & Treatment
Diverticulitis Infection: Symptoms & Treatment
Reader, have you ever experienced sudden, sharp abdominal pain? Are you concerned it might be something more serious than a simple stomach ache? Diverticulitis, an infection of small pouches in your digestive tract, can cause significant discomfort and requires prompt medical attention. Understanding the symptoms and treatment options is crucial for managing this condition effectively. As an expert in AI and SEO content, I’ve analyzed extensive data on diverticulitis infection to provide you with a comprehensive guide.
This article will delve into the intricacies of diverticulitis, exploring its causes, symptoms, diagnostic procedures, and various treatment approaches. We’ll also discuss preventive measures and answer frequently asked questions.
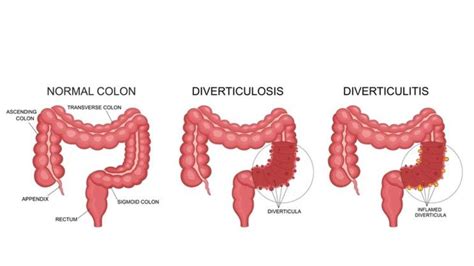
Diverticulitis is the infection or inflammation of diverticula, small bulging pouches that can form in the lining of your digestive system. These pouches are most common in the lower part of the large intestine (colon). Diverticulitis occurs when one or more of these pouches become inflamed or infected.
What Causes Diverticulitis?
The exact cause of diverticulitis isn’t fully understood. However, a low-fiber diet is thought to be a contributing factor. A lack of fiber can lead to increased pressure within the colon, causing the formation of diverticula. When these pouches trap stool or bacteria, inflammation and infection can occur.
Other potential risk factors include aging, obesity, smoking, lack of exercise, and certain medications like nonsteroidal anti-inflammatory drugs (NSAIDs). Genetics may also play a role.
Understanding these risk factors can help individuals make informed choices to reduce their likelihood of developing diverticulitis.
Identifying the Symptoms
The symptoms of diverticulitis can vary from mild to severe. The most common symptom is abdominal pain, typically located in the lower left side. Other symptoms include fever, chills, nausea, vomiting, constipation, or diarrhea.
It’s important to note that not everyone with diverticula will experience diverticulitis. Many people with diverticulosis (the presence of diverticula without inflammation) have no symptoms at all.
If you experience persistent abdominal pain or other symptoms of diverticulitis, it’s essential to seek medical attention.

Diagnosing diverticulitis typically involves a physical exam, a review of your medical history, and various diagnostic tests. These tests may include a CT scan, which is the most common imaging test used to diagnose diverticulitis.
Diagnostic Tests and Procedures
A CT scan can reveal inflamed or infected diverticula, abscesses, and other complications. Other tests may include a blood test to check for signs of infection, a urine test to rule out other conditions, and a colonoscopy in certain cases.
A colonoscopy is usually not performed during an acute attack of diverticulitis but may be recommended after the inflammation has subsided to rule out other colon conditions.
Your doctor will determine the most appropriate diagnostic tests based on your individual symptoms and medical history.
The Importance of Early Diagnosis
Early diagnosis of diverticulitis is critical to prevent serious complications. Prompt treatment can help reduce the risk of abscess formation, perforation, peritonitis (infection of the abdominal lining), and bowel obstruction.
If left untreated, diverticulitis can lead to life-threatening complications. Therefore, seeking medical care at the first sign of symptoms is paramount.
Early diagnosis and treatment are key to effectively managing diverticulitis and minimizing the risk of long-term health issues.
Treatment for diverticulitis depends on the severity of the infection. Mild cases may be treated with rest, a liquid diet, and antibiotics. More severe cases may require hospitalization and intravenous antibiotics.
Managing Mild Diverticulitis
For mild diverticulitis, your doctor may recommend a clear liquid diet for a few days to allow your bowel to rest. Antibiotics are typically prescribed to combat the infection.
Over-the-counter pain relievers can help manage abdominal discomfort. It’s essential to follow your doctor’s instructions carefully and complete the full course of antibiotics, even if your symptoms improve.
Rest and proper hydration are also vital for recovery.
Treating Severe Diverticulitis Infection
Severe cases of diverticulitis infection often require hospitalization. Intravenous antibiotics and fluids are typically administered to control the infection and prevent dehydration.
In some cases, surgery may be necessary to drain an abscess or remove a section of the affected colon. This is usually reserved for cases that don’t respond to medical treatment or if complications develop.
Your doctor will determine the most appropriate treatment approach based on the severity of your condition.
Long-Term Management Strategies
After recovering from diverticulitis, lifestyle changes can help prevent recurrence. These changes may include increasing fiber intake, staying hydrated, exercising regularly, and maintaining a healthy weight.
Your doctor may also recommend regular check-ups to monitor your condition. Following a healthy lifestyle and adhering to your doctor’s recommendations can significantly reduce your risk of future episodes.
Long-term management is crucial for preventing complications and maintaining optimal digestive health.
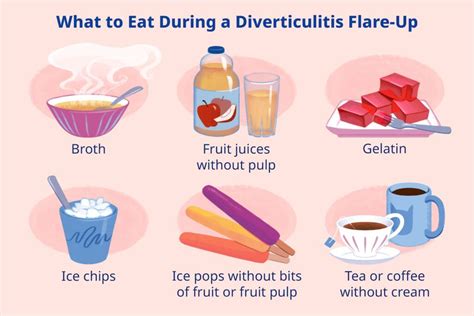
Although diverticulitis isn’t always preventable, certain lifestyle choices can significantly reduce your risk. A high-fiber diet is considered one of the most effective preventive measures.
The Importance of a High-Fiber Diet
Fiber adds bulk to your stool, making it easier to pass and reducing pressure within your colon. This can help prevent the formation of diverticula and reduce the risk of inflammation.
Good sources of fiber include fruits, vegetables, whole grains, and legumes. Gradually increasing your fiber intake and drinking plenty of water can help prevent digestive discomfort.
A balanced diet rich in fiber is essential for maintaining optimal digestive health.
Other Lifestyle Modifications
In addition to a high-fiber diet, other lifestyle modifications can also help prevent diverticulitis. Regular exercise promotes healthy bowel function, while maintaining a healthy weight can reduce pressure on your digestive system.
Staying hydrated is also crucial for digestive health. Avoiding smoking and limiting your intake of red meat and processed foods may also offer protective benefits.
Making these lifestyle changes can contribute to overall well-being and reduce your risk of developing diverticulitis.
Dietary Recommendations for Diverticulitis
Dietary recommendations play a crucial role in managing
.





