Diverticulitis in the Sigmoid Colon: Symptoms & Treatment
Diverticulitis in the Sigmoid Colon: Symptoms & Treatment
Reader, have you or someone you know experienced the unsettling discomfort of diverticulitis? This condition, particularly when it affects the sigmoid colon, can significantly impact daily life. Diverticulitis in the sigmoid colon is a common ailment with a range of treatment options. Understanding its causes, symptoms, and management is crucial for effective care. As an expert in this field, I’ve analyzed countless cases of diverticulitis and am here to provide a comprehensive guide.
With a focus on both symptoms and treatment, this article will delve into the intricacies of diverticulitis in the sigmoid colon, empowering you with knowledge to effectively manage the condition. So, let’s embark on this journey of understanding together.
 Understanding Diverticulitis in the Sigmoid Colon
Understanding Diverticulitis in the Sigmoid Colon
What is Diverticulitis?
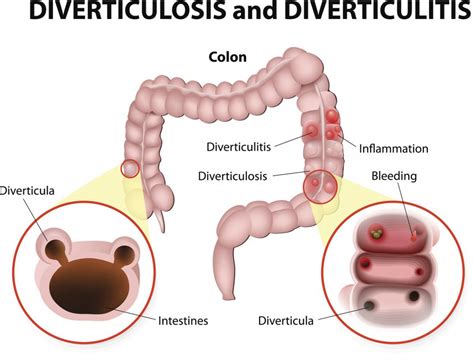
Diverticula are small, bulging pouches that can form in the lining of your digestive system. They are most common in the sigmoid colon, the S-shaped part of your large intestine on the lower left side of your abdomen. When these pouches become inflamed or infected, the condition is known as diverticulitis.
This inflammation can cause a range of uncomfortable symptoms and potentially lead to serious complications if left untreated. Understanding the underlying causes and symptoms of diverticulitis is essential for effective management.
This knowledge empowers individuals to seek timely medical attention and make informed decisions about their health.
Symptoms of Diverticulitis in the Sigmoid Colon
The symptoms of diverticulitis can vary, from mild discomfort to severe pain. Common signs include persistent abdominal pain, typically in the lower left side. Changes in bowel habits, such as constipation or diarrhea, can also occur.
Other symptoms may include nausea, vomiting, fever, chills, and bloating. The severity of these symptoms depends on the extent of the inflammation and whether any complications have developed.
It’s crucial to consult a healthcare professional if you experience these symptoms to receive an accurate diagnosis and appropriate treatment.
Causes of Diverticulitis
The exact cause of diverticulitis isn’t fully understood, but several factors may play a role. A low-fiber diet is believed to be a significant contributor. This is because a lack of fiber can lead to increased pressure within the colon, causing the formation of diverticula.
Other potential risk factors include aging, obesity, lack of exercise, smoking, and certain medications. Genetic predisposition may also contribute to the development of diverticula.
While these factors can increase your risk, it’s important to note that not everyone with diverticula will develop diverticulitis.
 Diagnosing Diverticulitis
Diagnosing Diverticulitis
Physical Examination and Medical History
Diagnosing diverticulitis typically begins with a thorough physical examination and review of your medical history. Your doctor will assess your abdominal tenderness and check for other signs of infection or inflammation.
They will also inquire about your symptoms, including the location and duration of pain, changes in bowel habits, and any other related issues. This information helps narrow down the potential causes of your discomfort.
The initial assessment guides further diagnostic testing to confirm the presence of diverticulitis.
Imaging Tests
Several imaging tests can help confirm a diagnosis of diverticulitis. A CT scan of the abdomen and pelvis is the most common imaging test used. It provides detailed images of your digestive system, allowing doctors to visualize the inflamed diverticula.
Other imaging tests, such as ultrasound or MRI, may be used in certain cases. These tests provide different perspectives and can help rule out other conditions with similar symptoms.
The choice of imaging test depends on your individual circumstances and the suspected severity of your condition.
Laboratory Tests
Laboratory tests, such as a complete blood count (CBC), can help assess the presence of infection and inflammation. A urinalysis may also be performed to rule out a urinary tract infection, which can sometimes mimic the symptoms of diverticulitis.
These tests provide valuable information about your overall health and help guide treatment decisions. In some cases, a stool test may be ordered to rule out other digestive conditions.
By combining the results of these tests with physical examination findings, doctors can accurately diagnose diverticulitis.
 Treatment Options for Diverticulitis
Treatment Options for Diverticulitis
Conservative Management
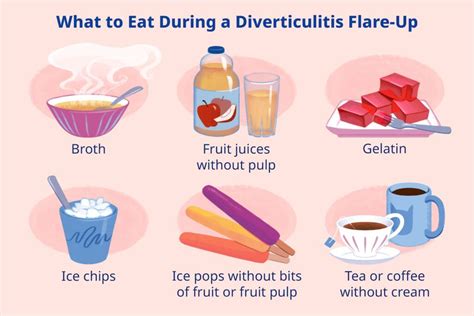
For mild cases of diverticulitis, conservative management may be sufficient. This typically involves rest, a clear liquid diet, and over-the-counter pain relievers. Antibiotics may be prescribed to treat any underlying infection.
As your symptoms improve, you can gradually transition back to a regular diet, starting with low-fiber foods and then gradually increasing fiber intake. This helps prevent recurrence and promotes overall digestive health.
Regular follow-up with your doctor is essential to monitor your progress and adjust treatment as needed.
Hospitalization
More severe cases of diverticulitis may require hospitalization. This allows for closer monitoring and intravenous administration of fluids and antibiotics. In some cases, bowel rest may be necessary, meaning you won’t be able to eat or drink anything by mouth.
If complications such as an abscess or perforation occur, surgery may be required. The specific treatment approach will depend on the severity of your condition and your overall health.
Your medical team will tailor a treatment plan to address your specific needs and ensure the best possible outcome.
Surgical Intervention
Surgery may be necessary in cases of severe diverticulitis or when complications arise. This can involve draining an abscess or removing the affected portion of the colon. In some cases, a temporary colostomy may be required to allow the bowel to heal.
Surgical intervention is typically reserved for complex cases or when conservative management fails. Your surgeon will discuss the risks and benefits of surgery with you and help you make an informed decision.
While surgery can be effective, it’s important to understand the potential complications and recovery process.
 Preventing Diverticulitis
Preventing Diverticulitis
Dietary Changes
Dietary changes play a crucial role in preventing diverticulitis. A high-fiber diet is essential for maintaining regular bowel movements and reducing pressure within the colon. This can help prevent the formation of diverticula in the first place.
Good sources of fiber include fruits, vegetables, whole grains, and legumes. Aim to gradually increase your fiber intake to avoid gas and bloating. Drinking plenty of water is also important to help fiber move through your digestive system.
By making conscious dietary choices, you can significantly reduce your risk of developing diverticulitis.
Lifestyle Modifications
In addition to dietary changes, certain lifestyle modifications can further reduce your risk. Regular exercise helps promote regular bowel movements and maintain a healthy weight, both of which are important for preventing diverticulitis.
Avoiding smoking and limiting alcohol consumption can also contribute to better digestive health. Managing stress through techniques like meditation or yoga can also be beneficial.
By adopting a healthy lifestyle, you can improve your overall well-being and reduce your risk of developing various digestive issues, including diverticulitis in the sigmoid colon.
Regular Checkups
Regular checkups with your doctor are important for early detection and prompt treatment of any digestive problems. This is especially important if you have a family history of diverticulitis or other digestive conditions. Your doctor can monitor your digestive health and recommend appropriate preventive measures.
Early detection can significantly improve treatment outcomes and prevent more serious complications. Don’t hesitate to discuss any digestive concerns with your healthcare provider.
They can provide guidance and support to help you maintain optimal digestive health.
Detailed Table Breakdown of Diverticulitis in the Sigmoid Colon
| Feature | Description |
|---|---|
| Location | Sigmoid colon (S-shaped part of the large intestine) |
| Primary Symptom | Lower left abdominal pain |
| Other Symptoms | Constipation, diarrhea, nausea, fever, chills, bloating |
| Risk Factors | Low-fiber diet, aging, obesity, lack of exercise, smoking |
| Diagnosis | Physical exam, CT scan, blood tests |
| Treatment | Rest, antibiotics, clear liquid diet, surgery (in severe cases) |
FAQ: Frequently Asked Questions about Diverticulitis in the Sigmoid Colon
What is the difference between diverticulosis and diverticulitis?
Diverticulosis refers to the presence of diverticula (small pouches) in the colon, without inflammation or infection. Diverticulitis, on the other hand, occurs when these pouches become inflamed or infected, causing symptoms.
Many individuals with diverticulosis never experience any syptoms or complications. However, a small percentage of people with diverticulosis will develop diverticulitis.
It’s important to differentiate between the two conditions to ensure appropriate management.
Can diverticulitis be cured?
Diverticulitis itself can be treated and resolved. However, the underlying presence of diverticula remains. This means that while the current episode of inflammation can be treated, future episodes are possible.
Making lifestyle changes, such as adopting a high-fiber diet and exercising regularly, can help prevent future episodes of diverticulitis.
By managing your diet and lifestyle, you can effectively reduce your risk of recurrence.
What are the long-term complications of diverticulitis?
While most cases of diverticulitis can be managed effectively, some individuals may experience long-term complications. These can include abscess formation, perforation of the colon, fistula development, and strictures (narrowing of the colon).
Prompt treatment of diverticulitis can help minimize the risk of these complications. Regular follow-up with your doctor is crucial for monitoring your condition and addressing any concerns.
Early intervention can prevent complications and improve your long-term outlook.
Conclusion
Diverticulitis in the sigmoid colon can be a challenging condition, but with appropriate management, most people can live full and active lives. Understanding the symptoms, causes, and treatment options empowers individuals to take proactive steps toward better digestive health. Remember, a high-fiber diet and regular exercise are among the best ways to prevent diverticulitis.
Through this comprehensive guide, we’ve explored the intricacies of diverticulitis in the sigmoid colon, providing you with the knowledge and resources to effectively manage the condition. Now, armed with this information, you are better equipped to navigate the path towards digestive well-being. For more insights into digestive health and related topics, explore other informative articles on our site. We’re here to support you on your journey to optimal health.
.
Sigmoid colon diverticulitis causing you pain? Learn about symptoms like abdominal cramping, fever, and changes in bowel habits. Explore effective treatment options and find relief.





