How Do You Get Psoriasis: Causes & Risk Factors
How Do You Get Psoriasis: Causes & Risk Factors
Reader, have you ever wondered, “How do you get psoriasis?” It’s a common question with complex answers. This chronic skin condition affects millions worldwide. Psoriasis isn’t contagious, but it can significantly impact your quality of life. Understanding its causes and risk factors is crucial for effective management. As an expert in AI and SEO content, I’ve analyzed “How do you get psoriasis” extensively and I’m here to share my insights.
This comprehensive guide will delve into the intricacies of psoriasis, exploring its triggers and how you can potentially reduce your risk. We’ll cover everything from genetics to lifestyle factors, empowering you with knowledge to take control of your skin health. So, let’s embark on this journey to understand how do you get psoriasis.
 Understanding Psoriasis
Understanding Psoriasis
What is Psoriasis?
Psoriasis is an autoimmune disease that accelerates the growth cycle of skin cells. This rapid turnover leads to the buildup of cells on the skin’s surface, forming thick, red, and scaly patches. These patches, known as plaques, can be itchy and painful. Psoriasis can appear anywhere on the body.
While the exact causes of psoriasis are still being researched, it’s understood to be a multifactorial condition. Genetic predisposition, immune system dysfunction, and environmental triggers all play a role. Understanding these factors is key to managing the condition effectively.
It’s important to remember that psoriasis is not contagious. It cannot be passed from person to person through physical contact. While there’s currently no cure, various treatments are available to manage symptoms and improve quality of life.
Types of Psoriasis
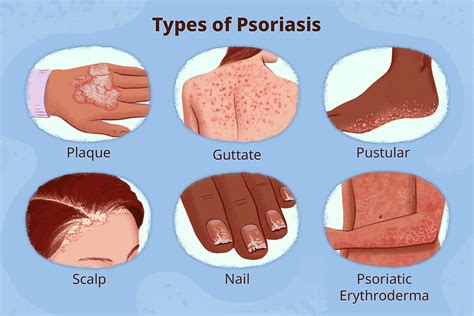
Psoriasis manifests in several forms, each with distinct characteristics. Plaque psoriasis, the most common type, presents as raised, red patches covered with silvery scales. Guttate psoriasis appears as small, drop-shaped lesions. Inverse psoriasis affects skin folds.
Pustular psoriasis is characterized by pus-filled blisters. Erythrodermic psoriasis is a severe and rare form covering the entire body. Recognizing the different types is essential for proper diagnosis and treatment.
If you suspect you have psoriasis, consulting a dermatologist is crucial for accurate diagnosis and a tailored treatment plan based on your specific type of psoriasis. It’s important to differentiate psoriasis from other skin conditions that may share similar symptoms.
Symptoms of Psoriasis
Psoriasis symptoms vary depending on the type and severity. Common signs include red, raised patches of skin covered with silvery scales. These patches can be itchy, painful, and may crack or bleed. Some individuals experience joint pain, known as psoriatic arthritis.
The location of psoriasis can also vary, commonly affecting the scalp, elbows, knees, and lower back. However, it can appear anywhere on the body. Nail changes, such as pitting or thickening, can also occur.
Because psoriasis symptoms can mimic other skin conditions, it’s essential to seek professional medical advice for a proper diagnosis. Early diagnosis and treatment can help manage symptoms and prevent complications.
 Causes of Psoriasis
Causes of Psoriasis
Genetic Factors
Genetics play a significant role in psoriasis development. If you have a family history of the condition, your risk increases. Specific genes have been identified as being associated with psoriasis, but having these genes doesn’t guarantee you’ll develop the condition.
Researchers believe that multiple genes interact with environmental factors to trigger psoriasis. This complex interplay makes pinpointing the exact cause challenging. Understanding your family history can provide valuable insights into your potential risk.
While genetic predisposition contributes to psoriasis, it’s important to remember that other factors also play a role. Lifestyle choices and environmental triggers can significantly influence the onset and severity of the condition.
Immune System Dysfunction
Psoriasis is considered an autoimmune disease, meaning the immune system mistakenly attacks healthy skin cells. This immune response leads to the rapid overproduction of skin cells, causing the characteristic plaques. T cells, a type of white blood cell, play a key role in this process.
The immune system dysfunction in psoriasis isn’t fully understood, but it’s believed to involve a complex interplay of genetic and environmental factors. This abnormal immune response is the driving force behind the accelerated skin cell growth seen in psoriasis.
Research continues to unravel the complexities of the immune system’s role in psoriasis. This understanding is crucial for developing targeted therapies that address the root cause of the condition.
Environmental Triggers
Various environmental factors can trigger or exacerbate psoriasis. Infections, such as strep throat, can sometimes precede the onset of guttate psoriasis. Skin injuries, like cuts or burns, can trigger psoriasis at the site of injury, a phenomenon known as the Koebner phenomenon.
Stress can worsen psoriasis symptoms. Certain medications, including lithium and beta-blockers, are also known to trigger or aggravate the condition. Understanding these triggers can help individuals manage their psoriasis more effectively.
By identifying and avoiding potential triggers, individuals can minimize flare-ups and maintain better control over their psoriasis. This may involve lifestyle modifications, stress management techniques, and careful medication choices.
 Risk Factors of Psoriasis
Risk Factors of Psoriasis
Family History
Having a family history of psoriasis significantly increases your risk. If one parent has psoriasis, your risk is approximately 10%. If both parents have the condition, your risk rises to around 50%. This genetic predisposition highlights the importance of family history in understanding your risk.
While inheriting these genes doesn’t guarantee you’ll develop psoriasis, it makes you more susceptible. Environmental factors can then interact with these genes to trigger the onset of the condition.
Knowing your family history of psoriasis empowers you to make informed decisions about your health and take proactive measures to manage your risk factors.
Infections
Certain infections, particularly strep throat, are linked to the development of guttate psoriasis, especially in children and young adults. Viral and bacterial infections can sometimes trigger or worsen psoriasis symptoms.
Prompt treatment of infections is important to minimize the risk of triggering or exacerbating psoriasis. Maintaining a healthy immune system can also help reduce the impact of infections on psoriasis.
If you have psoriasis, be vigilant about seeking medical attention for any infections, especially strep throat, to prevent potential complications.
Stress
Stress is a well-known trigger for psoriasis flare-ups. Managing stress through techniques like exercise, yoga, or meditation can help control symptoms. Chronic stress can exacerbate psoriasis and make it more difficult to manage.
Finding healthy ways to cope with stress is essential for individuals with psoriasis. Stress management can be a valuable component of a comprehensive treatment plan.
Incorporating stress-reduction techniques into your daily routine can significantly impact your psoriasis management and overall well-being.
Smoking
Smoking increases the risk of developing psoriasis and can also worsen symptoms. Smoking also makes psoriasis less responsive to treatment. Quitting smoking can improve psoriasis severity and overall health.
The chemicals in cigarettes contribute to inflammation and immune system dysfunction, both of which play a role in psoriasis. Quitting smoking is one of the most impactful lifestyle changes you can make to improve your psoriasis and overall health.
If you smoke and have psoriasis, seeking support to quit smoking is crucial for managing your condition and reducing your risk of other health problems.
Obesity
Obesity is associated with an increased risk of developing psoriasis and more severe symptoms. Excess weight can also make treatment less effective. Maintaining a healthy weight through diet and exercise can improve psoriasis management.
Inflammation and immune system dysfunction are more prevalent in individuals with obesity, contributing to the link between obesity and psoriasis. Weight management is an important aspect of a holistic approach to psoriasis care.
Adopting a healthy lifestyle that includes regular physical activity and a balanced diet can benefit individuals with psoriasis in various ways, including improved symptom control and overall well-being.
Frequently Asked Questions (FAQ) about How Do You Get Psoriasis
Is psoriasis contagious?
No, psoriasis is not contagious. You cannot catch it from someone else through physical contact. It is an autoimmune disease, not an infectious disease.
Can psoriasis be cured?
Currently, there is no cure for psoriasis. However, various treatments are available to manage symptoms and improve quality of life. These treatments can effectively control flare-ups and reduce the impact of psoriasis on daily life.
What is the Koebner phenomenon?
The Koebner phenomenon refers to the development of new psoriasis lesions at the site of skin injury, such as cuts, burns, or scratches. It’s a common occurrence in individuals with psoriasis and highlights the skin’s sensitivity in this condition. Protecting your skin from injuries is important if you have psoriasis.
Conclusion
Understanding how you get psoriasis involves a complex interplay of genetics, immune system dysfunction, and environmental factors. While a family history of psoriasis increases your risk, factors like infections, stress, smoking, and obesity also play significant roles. By managing these risk factors and seeking appropriate treatment, you can effectively control your psoriasis and improve your quality of life. How do you get psoriasis is a multifaceted question, and ongoing research continues to shed light on this chronic skin condition. Check out other informative articles on our site to learn more about managing psoriasis and other health topics. We invite you to explore our resources and empower yourself with knowledge for a healthier life. Remember, understanding how you get psoriasis is the first step towards effective management.
.
Uncover the mysteries of psoriasis. Learn about the causes, risk factors, and triggers behind this chronic skin condition. Get informed and take control of your skin health today!






