Best Foods for Diverticulitis: Diet Guide
Best Foods for Diverticulitis: Diet Guide
Reader, have you ever wondered what the best foods for diverticulitis are? Managing diverticulitis through diet can be challenging, but it’s crucial for preventing flare-ups. Understanding the right foods to eat and avoid can significantly impact your comfort and overall health. By making informed dietary choices, you can navigate diverticulitis with confidence and minimize discomfort. As an experienced SEO blog writer specializing in AI and SEO content, I’ve analyzed countless resources on the best foods for diverticulitis to help you achieve optimal digestive health.
Throughout this guide, we’ll explore evidence-based strategies for creating a diverticulitis-friendly diet. We’ll uncover which foods can soothe your symptoms and which ones to steer clear of. This comprehensive guide is designed to empower you with the knowledge you need to make informed choices about your diet.
 Understanding Diverticulitis
Understanding Diverticulitis
What is Diverticulitis?
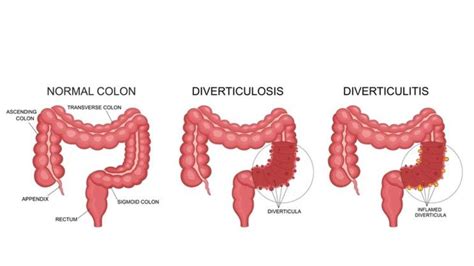
Diverticulitis is a condition affecting the digestive system, specifically the large intestine. It occurs when small pouches, called diverticula, form in the lining of the colon and become inflamed or infected. These pouches are typically harmless but can cause significant discomfort and health issues when inflamed.
Symptoms of diverticulitis can range from mild to severe, including abdominal pain, cramping, bloating, constipation, and fever. In severe cases, complications such as abscesses, perforations, and fistulas can develop, requiring immediate medical attention.
While the exact cause of diverticulitis isn’t fully understood, a low-fiber diet is believed to be a contributing factor. A diet lacking in fiber can lead to increased pressure in the colon, making it more susceptible to diverticula formation. Therefore, dietary modifications, particularly increasing fiber intake, play a crucial role in managing and preventing diverticulitis flare-ups.
The Role of Diet in Diverticulitis Management
Diet plays a pivotal role in managing diverticulitis. The foods we consume can either exacerbate or alleviate inflammation in the digestive tract. Choosing the right foods can help soothe symptoms, prevent flare-ups, and promote overall digestive health.
A diet rich in fiber is essential for managing diverticulitis. Fiber softens stool, making it easier to pass and reducing pressure on the colon. This helps prevent the formation of new diverticula and reduces the risk of existing ones becoming inflamed.
In addition to fiber, other dietary factors can influence diverticulitis. Staying hydrated by drinking plenty of water is essential for keeping the digestive system functioning smoothly. Probiotics, found in fermented foods like yogurt and kimchi, can also support gut health and reduce inflammation.
Identifying Trigger Foods
While dietary recommendations for diverticulitis have evolved, identifying personal trigger foods is crucial. Some individuals may find that certain foods, even healthy ones, exacerbate their symptoms. Keeping a food diary can help pinpoint these triggers and personalize your diet accordingly.
Common trigger foods for diverticulitis can include nuts, seeds, popcorn, and certain high-fiber foods. However, it’s important to remember that everyone’s tolerance is different. What triggers symptoms in one person may not affect another.
Working with a registered dietitian or healthcare professional can help you identify your specific trigger foods and develop a personalized diet plan that meets your individual needs. They can also provide guidance on safely increasing fiber intake and avoiding potential complications.
 Best Foods for Diverticulitis
Best Foods for Diverticulitis
High-Fiber Foods
Fiber is a cornerstone of a diverticulitis-friendly diet. Foods rich in fiber add bulk to the stool, promoting regular bowel movements and reducing pressure in the colon. This helps prevent the formation of new diverticula and reduces the risk of existing ones becoming inflamed or infected. Gradually increasing fiber intake is key to avoiding discomfort and bloating.
Excellent sources of fiber include fruits, vegetables, whole grains, and legumes. Fruits like apples, berries, and pears are not only packed with fiber but also provide essential vitamins and antioxidants. Vegetables such as broccoli, carrots, and spinach offer a variety of nutrients and fiber to support overall health.
Whole grains, including brown rice, quinoa, and oats, are a great way to incorporate more fiber into your diet. Legumes, such as lentils, beans, and chickpeas, are also excellent sources of fiber and plant-based protein. Adding these high-fiber foods to your diet can significantly improve digestive health and manage diverticulitis symptoms.
Probiotic-Rich Foods
Probiotics are beneficial bacteria that support gut health. They help maintain a healthy balance of microorganisms in the digestive tract, which can reduce inflammation and improve overall digestive function. Incorporating probiotic-rich foods into your diet can be particularly helpful during and after a diverticulitis flare-up.
Yogurt, kefir, kimchi, sauerkraut, and other fermented foods are excellent sources of probiotics. These foods introduce beneficial bacteria into the gut, helping to restore balance and reduce inflammation. Regular consumption of probiotic-rich foods can contribute to a healthier digestive system and potentially reduce the frequency and severity of diverticulitis flare-ups.
When choosing probiotic-rich foods, opt for those with live and active cultures. Check the labels to ensure the product contains beneficial bacteria strains. Incorporating a variety of probiotic-rich foods into your diet can provide a diverse range of beneficial bacteria for optimal gut health.
Hydration and Fluids
Staying hydrated is essential for everyone, but it’s particularly important for individuals with diverticulitis. Adequate fluid intake helps soften stool, making it easier to pass and reducing pressure on the colon. This can help prevent constipation, a common trigger for diverticulitis flare-ups.
Water is the best choice for hydration. Aim to drink at least eight glasses of water per day. Other fluids, such as herbal teas and clear broths, can also contribute to your daily fluid intake. Avoid sugary drinks, as they can exacerbate inflammation and worsen symptoms.
Staying hydrated is crucial for overall health and plays a vital role in managing diverticulitis. By ensuring you’re drinking enough fluids throughout the day, you can support healthy digestion and minimize the risk of flare-ups.
 Foods to Avoid with Diverticulitis
Foods to Avoid with Diverticulitis
Foods to Limit or Avoid
While a high-fiber diet is generally recommended for diverticulitis, certain high-fiber foods can sometimes exacerbate symptoms, especially during a flare-up. Nuts, seeds, and popcorn, although healthy in general, can sometimes irritate the digestive tract in some individuals with diverticulitis. It’s important to listen to your body and adjust your diet accordingly.
During a flare-up, it’s often advisable to follow a low-fiber diet temporarily to allow the digestive system to rest. This typically involves avoiding high-fiber foods like whole grains, fruits, and vegetables for a short period. Once the flare-up subsides, you can gradually reintroduce these foods into your diet.
Red meat, processed foods, and foods high in added sugars and unhealthy fats should also be limited or avoided. These foods can contribute to inflammation and worsen diverticulitis symptoms. Focusing on whole, unprocessed foods is key to managing diverticulitis and promoting overall health.
Managing Flare-Ups through Diet
During a diverticulitis flare-up, dietary modifications are crucial for managing symptoms and promoting healing. A clear liquid diet is often recommended to give the digestive system a break and reduce inflammation. This typically involves consuming clear broths, water, ice chips, and plain gelatin.
As symptoms improve, you can gradually transition to a low-fiber diet. This involves avoiding high-fiber foods like whole grains, fruits, and vegetables for a short period. Once the flare-up subsides, you can slowly reintroduce high-fiber foods back into your diet, paying close attention to any potential triggers.
Working with a healthcare professional or registered dietitian during a flare-up is essential. They can provide personalized guidance on managing your diet and ensure you’re getting the necessary nutrients while minimizing irritation to the digestive tract.
 Long-Term Dietary Strategies for Diverticulitis
Long-Term Dietary Strategies for Diverticulitis
Creating a Balanced Meal Plan
Creating a balanced meal plan is vital for long-term diverticulitis management. Focus on incorporating a variety of nutrient-rich foods, including high-fiber fruits, vegetables, whole grains, and lean proteins. This provides the body with the essential nutrients it needs for optimal health and digestive function.
Meal planning can also help ensure you’re getting enough fiber without overwhelming your digestive system. Gradually increasing fiber intake is key to avoiding discomfort and bloating. Start with smaller portions of high-fiber foods and gradually increase the amount as your body adjusts.
A balanced meal plan can help you maintain a healthy weight, which is important for managing diverticulitis. Excess weight can put extra pressure on the digestive system, increasing the risk of flare-ups. By incorporating a variety of nutrient-rich foods into your diet, you can support your overall health and manage diverticulitis effectively.
Working with a Dietitian
Consulting a registered dietitian is highly recommended for personalized guidance on the best foods for diverticulitis. A dietitian can assess your individual needs, identify potential trigger foods, and create a tailored meal plan that supports your digestive health.
They can also provide education on safely increasing fiber intake, managing flare-ups, and avoiding potential complications. A dietitian can help you navigate the complexities of a diverticulitis-friendly diet and empower you to make informed food choices.
Working with a dietitian is an investment in your long-term health and well-being. Their expertise can help you manage diverticulitis effectively and improve your overall quality of life.
Detailed Table Breakdown: Fiber Content of Common Foods
| Food | Fiber (grams per serving) |
|---|---|
| 1 cup cooked lentils | 15.6 |
| 1 cup cooked black beans | 15 |
| 1 medium pear with skin | 5.5 |
| 1 cup cooked oatmeal | 4 |
| 1 medium apple with skin | 4.4 |
| 1 cup cooked broccoli | 5.1 |
FAQ: Frequently Asked Questions About Diverticulitis and Diet
Can I eat nuts and seeds with diverticulitis?
The traditional advice was to avoid nuts and seeds, but current research suggests they don’t increase flare-up risk. Listen to your body; if they cause discomfort, avoid them. If not, enjoy them as part of a healthy diet.
Nuts and seeds are excellent sources of healthy fats, fiber, and protein, but some people with diverticulitis find they aggravate their symptoms. If you experience discomfort after eating nuts or seeds, it’s best to avoid them or limit your intake.
If you can tolerate nuts and seeds without any issues, include them as part of a balanced diet. They provide essential nutrients and can contribute to overall health.
Is popcorn allowed on a diverticulitis diet?
Similar to nuts and seeds, the current recommendation is not to restrict popcorn unless it causes you discomfort. Popcorn is a whole grain and provides fiber, but its hull can irritate sensitive digestive systems.
If you experience discomfort after eating popcorn, it’s best to avoid it. There are plenty of other high-fiber foods you can enjoy without aggravating your symptoms.
If popcorn doesn’t bother you, enjoy it in moderation as part of a balanced diet. Just be mindful of added butter, salt, or excessive amounts of oil, as these can be detrimental to your health.
What should I eat during a diverticulitis flare-up?
During a flare-up, focus on easily digestible, low-fiber foods. Clear liquids like broth, water, and popsicles are typically recommended initially. As symptoms improve, gradually transition to a low-fiber diet, followed by a gradual return to your regular high-fiber diet as tolerated.
During a flare-up, your digestive system needs time to rest and heal. Avoid high-fiber foods, nuts, seeds, and any other foods that you suspect may trigger your symptoms. Focus on hydrating and providing your body with easily digestible nutrients.
As your symptoms improve, you can gradually reintroduce foods into your diet. Start with low-fiber options and gradually increase fiber intake as tolerated. Listen to your body and avoid any foods that cause discomfort.
Conclusion
Therefore, managing diverticulitis through diet involves choosing the best foods for diverticulitis to prevent flare-ups and maintain long-term digestive health. By understanding which foods to embrace and which to avoid, you can significantly impact your well-being.
Navigating the best foods for diverticulitis journey requires a combination of general dietary knowledge and personalized strategies. Remember that your digestive health is unique, so what works for one person might not work for another. Be sure to check out other articles on our site for more valuable information and empower yourself to take control of your digestive health. Prioritize a balanced, fiber-rich diet, stay hydrated, and consult with a healthcare professional for personalized guidance.
.
Soothe diverticulitis flares with the right foods. This guide explores the best and worst foods for managing your symptoms and preventing future episodes. Learn about high-fiber options, low-fiber choices for flare-ups, and foods to avoid.





