Diverticulitis: How Do You Get It?
Diverticulitis: How Do You Get It?
Reader, have you ever wondered about the mysterious ailment known as diverticulitis? And how exactly does one acquire this often painful condition? Diverticulitis is more common than you think, affecting a significant portion of the population, especially as they age. Understanding its root causes can empower you to make informed choices about your health. As an experienced health writer, I have analyzed countless studies and medical opinions on diverticulitis.
I’ve poured over the latest research to bring you the most comprehensive guide on the development of this condition. So, let’s dive in and demystify diverticulitis, exploring its causes, symptoms, and how you can minimize your risk.
 Understanding Diverticulitis
Understanding Diverticulitis
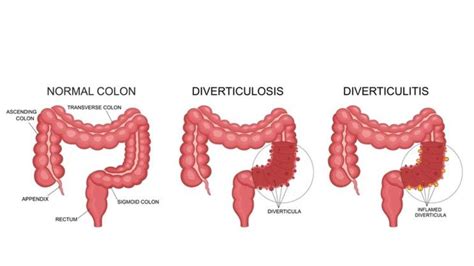
What are Diverticula?
Diverticula are small, bulging pouches that can form in the lining of your digestive system. They’re most common in the lower part of the large intestine (colon). Diverticula themselves are usually harmless and often don’t cause any noticeable symptoms. Many people have diverticula and never even know it.
However, these small pouches can become inflamed or infected. This leads to the painful condition known as diverticulitis. This inflammation can cause a range of uncomfortable symptoms, from abdominal pain to fever and changes in bowel habits.
Understanding the difference between diverticula and diverticulitis is crucial. While having diverticula isn’t necessarily a cause for concern, developing diverticulitis requires medical attention. This distinction helps in understanding how diverticulitis develops.
What Causes Diverticula to Form?
The exact cause of diverticula formation isn’t completely understood. However, a leading theory points to a lack of fiber in the diet. A low-fiber diet can lead to increased pressure inside the colon.
This increased pressure makes the colon work harder to move stool through. Over time, this strain can cause weak spots in the colon wall to bulge outward, forming diverticula. Think of it like a balloon being inflated too much – eventually, weak spots will start to protrude.
Other contributing factors may include aging, genetics, a sedentary lifestyle, smoking, obesity, and certain medications. These factors can weaken the colon wall or alter gut motility, increasing the likelihood of diverticula formation.
How Does Diverticulitis Develop?
Diverticulitis occurs when one or more of these diverticula become inflamed or infected. This can happen when stool or bacteria become trapped within the pouches. This trapped material can irritate the lining of the diverticula, leading to inflammation.
In some cases, the trapped material can even cause a small tear in the diverticulum wall. This tear allows bacteria to escape into the surrounding tissues, triggering an infection. The severity of diverticulitis can range from mild inflammation to a serious infection requiring hospitalization.
Prompt medical attention is important to prevent complications, such as abscess formation, peritonitis, or fistulas. Early diagnosis and treatment can significantly improve outcomes for individuals with diverticulitis. This is a key aspect of managing the condition.
 Risk Factors for Diverticulitis
Risk Factors for Diverticulitis
Age
Age is a significant risk factor for diverticulitis. As we age, the colon wall naturally weakens, making it more susceptible to diverticula formation.
The prevalence of diverticulosis, the presence of diverticula, increases dramatically after age 40. Diverticulitis, the inflamed or infected state, is more likely to occur in older individuals with diverticulosis.
While younger people can develop diverticulitis, it’s much less common. The aging process plays a significant role in the development of this condition.
Diet and Lifestyle
A low-fiber diet is considered a primary risk factor for developing diverticula, which can then lead to diverticulitis. Lack of fiber makes stool harder to pass, increasing pressure within the colon.
A sedentary lifestyle further contributes to this problem. Regular exercise helps promote healthy bowel movements and reduces strain on the colon. Smoking also increases the risk of diverticulitis.
Adopting a high-fiber diet and regular exercise can significantly reduce the risk of developing both diverticula and diverticulitis. These lifestyle changes are crucial for maintaining colon health.
Genetics and Other Factors
While lifestyle factors play a significant role, genetics also seem to influence the development of diverticulitis. Some individuals may have a genetic predisposition to weaker colon walls or altered gut motility.
Certain medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs), steroids, and opioids, can also increase the risk. These medications can irritate the lining of the digestive system, potentially contributing to inflammation.
Obesity is another risk factor, as it’s linked to increased pressure within the abdomen and changes in gut bacteria. Managing these factors can help reduce the risk of developing diverticulitis.
 Preventing Diverticulitis
Preventing Diverticulitis
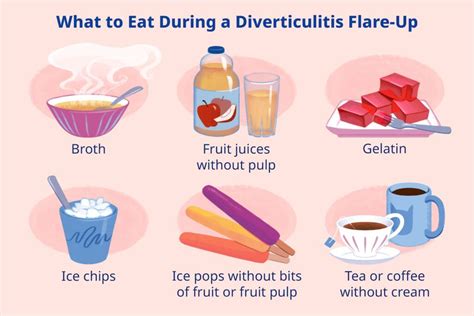
Increase Fiber Intake
One of the most effective ways to prevent diverticulitis is to increase your fiber intake. Fiber adds bulk to stool, making it easier to pass and reducing pressure on the colon. Aim for a daily intake of 25-30 grams of fiber.
Excellent sources of fiber include fruits, vegetables, whole grains, and legumes. Gradually increasing your fiber intake can help prevent digestive discomfort. Drink plenty of water along with fiber to aid in its effectiveness. This combination is key to good digestive health.
Choosing high-fiber foods is a proactive step towards preventing diverticulitis. In particular, dietary fiber and regular exercise can help maintain a healthy colon and prevent complications.
Regular Exercise
Regular physical activity helps improve bowel regularity and reduces strain on the colon. Aim for at least 30 minutes of moderate-intensity exercise most days of the week. This could include brisk walking, jogging, swimming, or cycling.
Exercise doesn’t have to be strenuous to be beneficial. Even simple activities like gardening or taking the stairs can contribute to better colon health. Find an activity you enjoy and make it part of your routine.
&l
.






