Ulcerative Colitis vs Diverticulitis: Key Differences
Ulcerative Colitis vs Diverticulitis: Key Differences
Reader, have you ever wondered about the distinctions between ulcerative colitis and diverticulitis? These two conditions, while both affecting the digestive system, present unique challenges and require distinct treatment approaches. Understanding the nuances of each is crucial for effective management. This comprehensive guide delves into the critical differences between ulcerative colitis and diverticulitis. As an expert in medical content creation, I’ve meticulously analyzed ulcerative colitis vs diverticulitis to provide you with accurate and invaluable insights.
In this in-depth exploration, we will dissect the symptoms, causes, diagnostic procedures, and treatment options for both conditions. This information will empower you to make informed decisions about your health or the health of loved ones. We’ll also touch upon the importance of early diagnosis and the role of lifestyle modifications in managing these conditions.
 Understanding Ulcerative Colitis
Understanding Ulcerative Colitis
What is Ulcerative Colitis?
Ulcerative colitis is a chronic inflammatory bowel disease (IBD) that affects the large intestine, specifically the colon and rectum. It causes inflammation and ulcers (sores) in the lining of the digestive tract. This inflammation can lead to a range of uncomfortable symptoms, including abdominal pain, cramping, and persistent diarrhea.
The disease often follows a relapsing-remitting course, meaning periods of active disease are interspersed with periods of remission. The severity of symptoms can vary significantly from person to person. Some individuals may experience mild discomfort, while others may have severe symptoms that significantly impact their quality of life. In some cases, untreated ulcerative colitis can even precipitate surgery.
While the exact cause of ulcerative colitis remains unknown, factors such as genetics, immune system dysfunction, and environmental triggers are thought to play a role. Early diagnosis and appropriate management are essential to minimize complications and improve outcomes for individuals with ulcerative colitis.
Symptoms of Ulcerative Colitis
The symptoms of ulcerative colitis can vary, ranging from mild to severe. Common symptoms include persistent diarrhea often accompanied by blood or pus, abdominal pain and cramping, and rectal pain or bleeding.
Other symptoms may include fatigue, weight loss, loss of appetite, and fever. The severity of symptoms is not consistent and can change over time. Some people may experience severe constant symptoms while some experience flare ups from time to time.
It’s important to note that these symptoms can also be indicative of other conditions. If you experience any of these symptoms, it’s crucial to consult a healthcare professional for proper diagnosis and treatment. Don’t hesitate to seek medical attention.
Treating Ulcerative Colitis
Treatment for ulcerative colitis focuses on managing inflammation, reducing symptoms, and preventing complications. Treatment options vary depending on the severity of the disease. Medications such as aminosalicylates, corticosteroids, and immunomodulators are commonly used to control inflammation.
In some cases, biologic therapies may be prescribed to target specific inflammatory pathways. For severe or refractory cases, surgery to remove the affected portion of the colon may be necessary. Lifestyle modifications, such as dietary changes and stress management, can also play a role in managing ulcerative colitis.
It’s important to work closely with a gastroenterologist to develop an individualized treatment plan that addresses your specific needs and symptoms. This plan needs to be tailored to your specific circumstances. Ulcerative colitis vs diverticulitis require different treatment approaches. Proactive treatment and symptom management are key for improving the quality of life for individuals with ulcerative colitis.
 Understanding Diverticulitis
Understanding Diverticulitis
What is Diverticulitis?
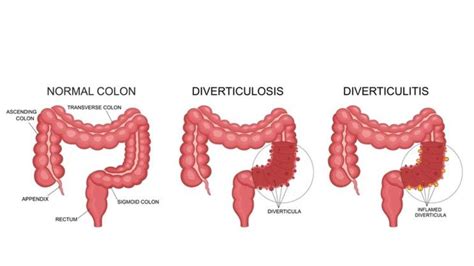
Diverticulitis is a condition that affects the digestive system, specifically the large intestine. It occurs when small pouches, called diverticula, that form in the lining of the intestine become inflamed or infected. These pouches are common, particularly in older adults, and are often asymptomatic.
However, when the diverticula become inflamed or infected, it leads to diverticulitis, which can cause significant abdominal pain, fever, and changes in bowel habits. The severity of diverticulitis can range from mild to life-threatening. Complications such as abscesses, perforations, and fistulas can occur. These complications can sometimes require surgery.
The exact cause of diverticulitis is not fully understood, but a low-fiber diet, aging, and genetics are thought to be contributing factors. Prompt diagnosis and appropriate treatment are crucial to prevent complications and manage diverticulitis effectively. Understanding ulcerative colitis vs diverticulitis can help in early detection and appropriate medical care.
Symptoms of Diverticulitis
The most common symptom of diverticulitis is abdominal pain, typically located in the lower left side. Other symptoms may include fever, chills, nausea, vomiting, constipation, or diarrhea. The severity of these symptoms can vary. Some cases may be mild and resolve without treatment, and in others, they may be severe, requiring hospitalization.
It’s important to note that some individuals with diverticulitis may not experience any noticeable symptoms. These individuals may only discover the condition during routine colonoscopies or other imaging studies. If you experience sudden or severe abdominal pain, especially accompanied by fever, it’s essential to seek medical attention immediately.
Prompt diagnosis and treatment can help prevent serious complications like abscesses, perforations, and fistulas. Accurate diagnosis is critical when comparing ulcerative colitis vs diverticulitis, as they present with some overlapping symptoms. Delaying medical care can exacerbate the condition.
Treating Diverticulitis
The treatment for diverticulitis depends on the severity of the condition. Mild cases may be managed with rest, a liquid diet, and antibiotics to clear the infection. More severe cases may require hospitalization, intravenous antibiotics, and pain management. In some cases, surgery may be necessary to drain abscesses or repair perforations.
For recurrent or complicated diverticulitis, surgical resection of the affected portion of the colon may be recommended. Lifestyle modifications, such as increasing fiber intake and staying hydrated, can also help prevent future episodes of diverticulitis.
It’s essential to follow your doctor’s recommendations carefully and complete the full course of antibiotics even if your symptoms improve. Understanding the differences between ulcerative colitis vs diverticulitis is crucial for tailoring the right treatment plan. Regular check-ups and adherence to prescribed treatments are vital for managing diverticulitis effectively. This helps prevent recurrence and improve long-term outcomes. Early diagnosis and proactive treatment contribute significantly to managing diverticulitis and improving the quality of life.
 Key Differences: Ulcerative Colitis vs Diverticulitis
Key Differences: Ulcerative Colitis vs Diverticulitis
While both ulcerative colitis and diverticulitis affect the digestive system, they are distinct conditions with different underlying causes, pathologies, and treatment approaches. Understanding these key differences is crucial for accurate diagnosis and effective management. This section will delve into the specific points of contrast between these two conditions, providing a clearer picture of ulcerative colitis vs diverticulitis.
This knowledge is essential for both patients and healthcare professionals. By highlighting the unique characteristics of each condition, we aim to empower individuals to make informed decisions about their health. Educating ourselves about these distinctions helps us better navigate the complexities of digestive health.
A thorough understanding of ulcerative colitis vs diverticulitis is imperative for appropriate medical care. Misdiagnosis can lead to ineffective treatments and potentially worsen the condition. With accurate knowledge, individuals can advocate for themselves and seek the right medical expertise.
Detailed Table Breakdown: Ulcerative Colitis vs Diverticulitis
| Feature | Ulcerative Colitis | Diverticulitis |
|---|---|---|
| Definition | Chronic inflammatory bowel disease affecting the colon and rectum. | Inflammation or infection of pouches (diverticula) in the lining of the large intestine. |
| Location | Colon and rectum (continuous inflammation). | Primarily the sigmoid colon (left lower abdomen). |
| Symptoms | Persistent diarrhea (often bloody), abdominal pain, rectal bleeding, fatigue. | Abdominal pain (usually left-sided), fever, chills, nausea, vomiting, constipation, or diarrhea. |
| Cause | Unknown, but likely a combination of genetic, immune, and environmental factors. | Likely related to a low-fiber diet, aging, and genetics. |
| Diagnosis | Colonoscopy, biopsy, blood tests, stool tests. | CT scan, blood tests, stool tests. |
| Treatment | Medications (aminosalicylates, corticosteroids, immunomodulators, biologics), surgery (in severe cases). | Antibiotics, pain relievers, liquid diet, surgery (for complications or recurrence). |
 The Importance of Early Diagnosis
The Importance of Early Diagnosis
Early Diagnosis: Ulcerative Colitis
Early diagnosis of ulcerative colitis is crucial for preventing complications and improving long-term outcomes. Early intervention can help control inflammation before it causes extensive damage to the colon. This helps maintain a better quality of life.
If you experience persistent digestive issues, don’t hesitate to consult a gastroenterologist. They can perform the necessary tests, including colonoscopies and biopsies, to confirm the diagnosis and initiate appropriate treatment. Don’t delay seeking medical attention if you suspect you may have ulcerative colitis.
Early and accurate diagnosis is essential for distinguishing ulcerative colitis vs diverticulitis and initiating the right treatment path. Prompt medical attention plays a vital role in managing the condition effectively. Delaying diagnosis can lead to more severe complications and a more challenging treatment journey.
Early Diagnosis: Diverticulitis
Early diagnosis of diverticulitis is essential to prevent potentially serious complications such as abscesses, perforations, and peritonitis. If you experience sudden, severe abdominal pain, especially in the lower left side, seek immediate medical attention. Prompt medical care can significantly improve the outcome.
A CT scan can confirm the diagnosis and determine the extent of inflammation. Early intervention with antibiotics and other supportive measures can help resolve the infection and prevent further complications. Recognizing the symptoms and promptly seeking medical care plays a vital role in managing diverticulitis successfully.
If you have risk factors for diverticulitis, such as a low-fiber diet and a family history of the condition, discuss preventive measures with your doctor. Understanding ulcerative colitis vs diverticulitis helps in making informed decisions about one’s health. Proactive discussions with healthcare professionals can lead to better health outcomes. Early diagnosis and intervention can make significant difference for both ulcerative colitis and diverticulitis.
Living with Ulcerative Colitis and Diverticulitis
Managing Ulcerative Colitis
Living with ulcerative colitis requires ongoing management to control symptoms and prevent flare-ups. Work closely with your gastroenterologist to develop a personalized treatment plan. This plan might include medications, lifestyle modifications, and regular monitoring.
Dietary changes, such as avoiding trigger foods and increasing fiber intake, can help manage symptoms. Stress management techniques, such as yoga and meditation, can also be beneficial. Support groups and online resources can provide emotional support and practical advice.
Understanding ulcerative colitis vs diverticulitis helps patients differentiate their specific needs and seek appropriate support. Active participation in managing one’s condition and seeking support leads to better health outcomes. Continuous communication between patients and healthcare providers is key for effective management of ulcerative colitis.
Managing Diverticulitis
Managing diverticulitis often involves lifestyle changes, including increasing fiber intake and staying adequately hydrated. These changes can help prevent the formation of new diverticula and reduce the risk of future episodes of diverticulitis.
Regular exercise and maintaining a healthy weight can also be beneficial. In some cases, your doctor may recommend prophylactic antibiotics to prevent recurrent infections. Understanding ulcerative colitis vs diverticulitis allows patients to focus on the specific management strategies for their condition.
Proactive engagement and consistent follow-up with healthcare providers contribute to improved health outcomes. Patients need to be actively involved in their care, understand their individual needs, and adhere to their treatment plans. This active participation promotes a stronger patient-physician relationship and improved management of diverticulitis.
FAQ: Frequently Asked Questions about Ulcerative Colitis and Diverticulitis
What are the key differences between ulcerative colitis and diverticulitis?
Ulcerative colitis is a chronic inflammatory bowel disease affecting the colon and rectum, while diverticulitis is an infection or inflammation of pouches in the large intestine.
Ulcerative colitis causes continuous inflammation, while diverticulitis affects specific pouches. Symptoms and treatment also differ. Understanding the distinction between ulcerative colitis vs diverticulitis is crucial for proper diagnosis and care.
Accurate diagnosis facilitates appropriate treatment and better management of each condition. Misdiagnosis can lead to ineffective treatments and potential complications. Therefore, it’s essential to seek professional medical advice for proper diagnosis and a tailored treatment plan.
Can you have both ulcerative colitis and diverticulitis?
While it’s rare, it is possible to have both ulcerative colitis and diverticulitis. However, these are distinct conditions with different underlying causes and pathophysiologies. Having one condition doesn’t necessarily increase the risk of developing the other.
If you experience symptoms suggestive of either condition, it’s crucial to consult a gastroenterologist for proper evaluation and diagnosis. Differentiating between ulcerative colitis vs diverticulitis is essential for targeted treatment. An accurate diagnosis is paramount for providing appropriate care.
Misdiagnosis can lead to inappropriate treatment and potentially harmful consequences. Therefore, seeking professional medical advice is crucial for determining the correct diagnosis and developing an effective treatment plan. It’s essential to work closely with your healthcare provider for accurate diagnosis and personalized care.
Conclusion
In conclusion, understanding the key differences between ulcerative colitis and diverticulitis is crucial for effective diagnosis and treatment. While both conditions affect the digestive system, they have distinct characteristics and require tailored approaches. Armed with this knowledge, you can better navigate the complexities of these conditions and seek appropriate medical care.
We’ve explored the various facets of ulcerative colitis vs diverticulitis, highlighting their unique symptoms, causes, and treatment options. This comprehensive guide aims to empower you with the information necessary to make informed decisions about your health or the health of loved ones. For further insights into digestive health topics, explore other informative articles on our site. We encourage you to delve deeper into ulcerative colitis vs diverticulitis to equip yourself with a thorough understanding. We are dedicated to providing valuable resources for your health journey.
.
Ulcerative colitis or diverticulitis? Learn the key differences in symptoms, causes, and treatments. Get the facts and understand your gut!





